Abstract
Background: Numerous studies have highlighted the inequitable access to medical and psychiatric care that people experiencing homelessness (PEH) face, yet the surgical needs of this population are not well understood. We sought to assess evidence describing surgical care for PEH and to perform a thematic analysis of the results.
Methods: Ovid MEDLINE, Embase, and Web of Science were searched using the terms “surgery” AND “homelessness.” Grey literature was also searched. We used a stepwise scoping review methodology, followed by thematic analysis using an inductive approach.
Results: We included 104 articles in our review. Studies were included from 5 continents; 63% originated in the United States. All surgical specialties were represented with varying surgical conditions and procedures for each. Orthopedic surgery (21%) was the most frequently reported specialty. Themes identified included characteristics of PEH receiving surgical care, homeless-to-housed participants, interaction with the health care system, educational initiatives, barriers and challenges, and interventions and future strategies.
Conclusion: We identified significant variation and gaps, representing opportunities for further research and interventions. Further addressing the barriers and challenges that PEH face when accessing surgical care can better address the needs of this population.
Homelessness is a major social and health-related concern globally. In Canada alone, there are 25 000–35 000 people experiencing homelessness (PEH) on any single night.1 The circumstances surrounding an individual’s homelessness are unique, complex, and multifactorial. Primary individual factors include poverty,2 adverse experiences in early childhood,3 mental health and substance use,2,4 personal history of violence, 5 and association with the criminal justice system.6 Structural factors reflect inadequate safety nets, including lack of affordable housing, reduced employment opportunities for low-skilled workers, low minimum wage, and no income support programs.7 Inherent systemic income inequality promotes homelessness, as countries with greater levels of income inequality also have higher rates of homelessness. 8 The COVID-19 pandemic further exacerbated the housing instability crisis through its negative impact on the economy and the reduced access to social services. Studies have noted an increase in PEH during the pandemic.9,10
The associations between experiencing homelessness and negative health outcomes are well documented. Individuals with mental health disorders are at a higher risk of homelessness, and a large proportion of PEH are also living with mental illness.11 Specifically, homelessness has been linked to schizophrenia,12 bipolar disorder,12 anxiety,13 posttraumatic stress disorder,13 and personality disorders.14 In addition, PEH are more likely to experience acute and chronic medical illnesses such as infectious diseases,15 skin and soft tissue infections,15 cardiovascular disease,16 diabetes, 17,18 and hypertension.18 The age-matched standardized mortality rates for PEH in high-income countries are typically 2–5 times those of the general population.15
Housing instability is associated with increased exposure to violence, assault, and unintentional injury,15,19 and PEH are overrepresented among populations with traumatic and exposure injuries such as traumatic brain injury,20 burns,21 and facial fractures,19 all of which are conditions that often require surgical care. The surgical needs of PEH are not well documented, yet housing status affects the approach to surgical care along its entire continuum from preoperative preparation to surgical decision-making and postoperative care.22
To date, there has been 1 scoping review on the topic of surgical care for PEH, which focused on the phases of care pertaining to operative management in the United States, United Kingdom, and Canada.22 To further investigate the surgical needs and state of surgical care for PEH, we sought in the present review to assess evidence describing surgical care for PEH and to perform a thematic analysis of the findings. Operative and nonoperative aspects of care that fall under the responsibilities of surgeons were specifically included.
Methods
We chose to perform a scoping review to identify the nature and extent of the literature on surgical care for PEH.23 The Arksey and O’Malley framework24 was followed, in addition to the select suggestions made by Levac and colleagues.25 A health research librarian was consulted to refine the research question and inform the search strategy.
Literature search
We searched Ovid MEDLINE, Embase, and Web of Science from database inception to Mar. 19, 2022. Table 1 shows the keywords and subject headings applied in each database. A forward snowballing strategy was also used to identify relevant literature from other published studies on this topic.22 The inclusion criteria were studies published in English that described a direct connection between surgical care and PEH. Studies that referred to dentistry, emergency/disaster response and refugees were excluded.
Search terms/MESH headings per database
One reviewer (C.P.) searched the grey literature with guidance from the Canadian Agency for Drugs and Technologies in Health (CADTH) Grey Matters checklist (2019).26 Sources included search engines, database searches, clinical practice guidelines, and health economics databases. The timeframe of the search was from Jan. 1, 2000, to Apr. 5, 2022, as a majority of the studies from the main literature were published in the 2000s. The main search terms were “homeless*,” “surg*,” and “operat*.”
Two independent reviewers (C.H., P.H.) screened the titles and abstracts of articles in duplicate according to the inclusion and exclusion criteria. Reviewers met at the beginning, midpoint, and final stages to discuss study selection and refine the search strategy if necessary. Interrater reliability was calculated using Cohen κ, with 0 representing no agreement and 1 representing perfect agreement.27 When conflict arose, a third reviewer (M.M.) was consulted to make the final decision. Full-text screening was done independently by the same 2 reviewers (C.H., P.H.). Covidence was used for text/abstract and full-text screening. 28
Data were extracted into a data collection form on Covidence by 2 reviewers (C.H., P.H.). The details of the extraction table were reviewed by all authors and edited before and during extraction as needed (Appendix 1, available at www.canjsurg.ca/lookup/doi/10.1503/cjs.004023/tab-related-content).
Data analysis
Included studies were assessed using a stepwise scoping review methodology and analyzed using descriptive statistics. Articles underwent thematic analysis using an inductive approach. The preliminary results were reviewed with an advisory panel including 3 physicians (2 surgeons and 1 shelter health physician) as well as a consultant with lived experience in homelessness. Feedback led to further search for guidelines from local and national organizations specific to surgical care for PEH. Further directions for research mentioned were included in the discussion.
Results
Literature search
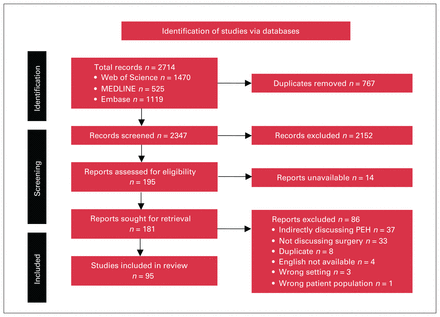
Our search produced 2714 studies, from which 95 studies were included (Figure 1 and Appendix 2, available at www.canjsurg.ca/lookup/doi/10.1503/cjs.004023/tab-related-content).29 Cohen κ was 0.72 for title/abstract screening, showing substantial agreement. An additional 4 studies were included from the grey literature search (Appendix 3, available at www.canjsurg.ca/lookup/doi/10.1503/cjs.004023/tab-related-content) and 5 from forward snowballing (Appendix 4, available at www.canjsurg.ca/lookup/doi/10.1503/cjs.004023/tab-related-content), giving this study a final sample of 104 articles.
Study selection based on the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020.29 PEH = people experiencing homelessness.
Most of the articles were published within the last 5 years (70/103 [68%]). Additionally, most of the studies were conducted in the United States (74/117 [63%]) and Canada (16/117 [14%]), with some studies occurring in more than 1 country. Publications from around the world were included, with articles from Kenya, Australia, and South Korea.
Half of the studies were retrospective chart reviews or retrospective cohort studies (52/104 [50%]). The second most frequent publications were abstracts from conference presentations (17/104 [16%]). Five studies used qualitative methods or participant-reported outcomes in the form of semistructured interviews and surveys. Of these, 4 investigated the opinions of physicians and other health care professionals (Table 2).30–34
List of study classification and corresponding number
Definition of homelessness
The definition of homelessness varied among studies (Table 3). Sixty-eight (65%) studies used the term “homelessness” without explanation or specific criteria for how a patient would be classified as experiencing homelessness. Thirty-six (35%) studies provided explicit definitions that ranged from using International Classification of Diseases (ICD-9/10) codes, no fixed address/shelter during registration in hospital, or expanded criteria to include the hidden homeless or those at risk of homelessness. A few studies had definitions that were vague, too broad, or not further elaborated by the authors. These findings are in keeping with the scoping review by Abel and colleagues, which also considered the definition of homelessness for the 23 articles that were included.22
Summary of definitions of homelessness among studies
Surgical procedures: prevalence and disparities
All surgical specialties were mentioned at least once within the 104 included articles (Appendix 1, Table 2). The most frequent surgical specialties pertaining to the care of PEH were orthopedic surgery (25/121 [21%]), plastic surgery (23/121 [19%]), and general surgery (20/121 [17%]).
A variety of conditions and procedures were described for each specialty (Table 4). Many discussed an increased prevalence of specific conditions and procedures among PEH (Table 5), albeit with some conflicting findings among studies.
Summary of surgical conditions, procedures, and associated studies described for each specialty
Surgical procedures and conditions with increased prevalence among PEH
Zuccaro and colleagues35 investigated surgical referrals for PEH at a hospital in Ottawa, Canada. The majority of surgical referrals at the study sites were for traumatic injuries, and the most frequently consulted service was orthopedic surgery followed by plastic surgery. 35 Titan and colleagues36 reported that PEH had more emergent procedures than individuals with housing. The surgeries were less complex, with shorter operation times but longer postoperative lengths of stay. They also found that PEH were more likely to have orthopedic surgeries.36 Goodwin and Brown37 reported similar results to those of Titan and colleagues, with PEH being more likely to experience trauma or deep tissue infection.37 Blakely and colleagues38 specified that in their cohort of trauma patients PEH experienced more penetrating trauma or assault, but had significantly fewer motor vehicle collisions and were less likely to have moderate or severe injury.38
Eight primary studies39–41,43–47 and 1 abstract42 noted that PEH received fewer operations than individuals with housing for orthopedic trauma injury, burns, eye surgery, valve surgery, and coronary artery bypass graft (CABG); however, findings related to CABG varied, with a study finding no significant difference.39–46 Another study described a lower prevalence of cesarean delivery among PEH.47 These studies noted this potential discrepancy but did not analyze the reasons behind it.
Cancer surgery for PEH
Three primary studies48–50 and 1 invited article51 described differences in operative management for cancer treatment among PEH. Festa and colleagues48 investigated women experiencing homelessness who were diagnosed with breast cancer. Most women received surgery as their first-line treatment (92%) but experienced significant delays (30–90 days) in receiving treatment. 48 For PEH with lung cancer, Suh and colleagues49 found that most PEH presented with advanced disease (78%) and passed away shortly after. Of the few PEH who presented with early-stage disease, 80% received curative surgery and all completed follow-up, with no recurrences or deaths.49 Additionally, Concannon and colleagues50 reported that PEH with lung cancer were less likely to undergo definitive treatment than patients with housing and experienced significant delays. A similar disparity was noted for pancreatic cancer, with Louie and colleagues51 reporting that patients who had pancreatic cancer and lower socioeconomic status were less likely to receive treatment compliant with National Comprehensive Cancer Network guidelines and were more likely to die from their cancer.
Three primary studies discussed the low cancer screening rates among PEH contributing to advanced disease upon presentation.31,52,53 With regards to colon cancer screening, for example, one-quarter of PEH surveyed had undergone colonoscopy in the last 10 years, and approximately three-quarters had never had a conversation with a health care provider about cancer screening.31,52 Bingham and colleagues53 found an overall disparity in the volume of published data about cancer screening and treatment in PEH.
Characteristics of PEH receiving surgical care
Four primary studies36,47,54,55 reported that the average age of PEH was younger than that of individuals with housing for similar disease processes, and another primary study38 reported fewer elderly PEH. Four primary studies47,56–58 also reported that PEH were more likely to be from racialized groups, including Black, Hispanic, and Native American.
Comorbidities
Surgical patients experiencing homelessness presented with multiple medical comorbidities, including infections (hepatitis C virus [HCV], HIV), cardiovascular conditions, lung disease, liver disease, osteoarticular disease, dermatologic disease, and head and neck conditions.47,59–63 These were all reported in primary studies57,59–61,63 and in 1 abstract.62 Titan and colleagues,36 in another primary study, noted that compared to patients with housing, PEH had fewer medical comorbidities but more psychiatric conditions for general, orthopedic, and vascular surgery admissions. Psychiatric comorbidities included mood disorders, psychotic disorders (reported in pregnancy), and high rates of substance use (smoking, alcohol use, intravenous drug use, multidrug use), reported in primary studies.58,64,65
Return to housing
Several primary studies reported that hospital admission was an opportunity to connect PEH with supportive services, including social work and housing assistance. A case series by Bennett and colleagues66 reported that 73% of PEH were permanently housed at final follow-up, and the other 17% were in temporary housing after receiving joint replacement surgery and extensive and coordinated medical and social services. The employment status of participants in their study also increased from 9% before surgery to 27% after surgery. There were minimal complications and no known readmissions, reoperations, infections, or deaths among the participants.66 Lawson and colleagues67 described a recuperative care pilot project for 23 PEH who were housed in a motel where the second most common admitting diagnosis (17%) was for postoperative recovery. The PEH were referred to services including case management, housing resources, and public assistance. Average length of stay was 37 days, and 22% were discharged to stable housing, whereas 30% had no identifiable housing at discharge.67 Podymow and colleagues68 documented a shelter-based convalescence unit where 12% of patients stayed postoperatively. In total, 60% of patients in the study applied for housing and 24.3% of them received housing.68
Interaction with health care systems
Within all phases of hospital treatment, increased obstacles were described in the care of PEH. These were documented in 5 primary studies,36,50,55,69,72 2 abstracts,37,38 a magazine article,70 and a thesis.71 After admission to hospital, PEH were reported to have a longer length of stay and to experience delayed discharge,36,37,45,55,69–71 although some studies found no difference.38,50 Kiwanuka and colleagues45 noted an increase in adjusted cost for inpatient care for PEH with burns, likely because of the significantly increased comorbidity burden in this population, such as psychiatric illness, chronic liver disease, chronic pulmonary disease, AIDS, and low body weight.45 Hwang and colleagues55 noted a similar increase in inpatient care costs for PEH on medical, psychiatric, and surgical services owing to increased length of stay for acute care and level of care days. Cai and colleagues69 also discussed how veterans experiencing homelessness were more likely to be discharged to some form of institutional care, primarily nursing homes; however, this is contradicted by the findings of Blakely and colleagues,38 who reported lower rates of discharge to rehabilitation or nursing facilities.38 Finally, PEH were reported to be more likely than people with housing to leave against medical advice.38,45,72
Outpatient follow-up
Reports regarding outpatient follow-up included 7 primary studies,35,41,50,59,73,75,76 a thesis,71 a systematic review,74 and an abstract.77 PEH were found to have fewer surgical visits and were less likely to be referred to outpatient care.73,74,59 They were also reported to be less likely to attend follow-up, with as many as 45%–55% missing their appointments. 35,41,59,71,74–77 Zuccaro and colleagues35 reported that just under half of referred patients attended at least 1 outpatient appointment and only one-third completed follow-up.35 Surprisingly, Concannon and colleagues50 found that PEH were not significantly more likely to miss appointments, but lost contact with the medical team twice as often as patients with housing owing to a combination of missed appointments, relocation, and admission to hospice. Kay and colleagues41 found that PEH who received an operation were more likely to return to the orthopedic clinic than nonoperative patients.
Visits to the emergency department
The retrospective chart review by Zuccaro and colleagues35 reported that the number of emergency department encounters per PEH for any reason was 7.9 visits over a period of 2 years, with a wide standard deviation of 1–106 visits. Other primary studies41,69,75,78 and a thesis71 noted an increased use of emergency departments by PEH compared to individuals with housing. In contrast, the retrospective chart review by Concannon and colleagues50 found no significant difference in the number of emergency department visits for PEH compared to counterparts with housing.
Readmission
Homelessness was described as a risk factor for readmission by several primary studies36,55,69,72,79 and a thesis.71 Titan and colleagues36 showed that the most notable predictor for readmission was discharge destination, as homeless veteran patients were significantly more likely to be readmitted when discharged to the community rather than a domiciliary or nursing home.36 Conversely, an abstract by Blakely and colleagues38 found no difference in 30-day readmission.
Complications
As with other outcomes, findings were inconsistent for complications among PEH. These were described in several primary studies,36,41,45,56,57,66,80,81,83,85–88 abstracts,38,42,82,84 and a thesis.71 Several studies reported that PEH were more likely to experience complications and treatment failure,71,80–84 whereas others reported no difference or the opposite.36,38,41,66 For example, 1 study found homelessness to be a risk factor for Methicillin-resistant Staphylococcus aureus (MRSA) in soft tissue infection, while another study found homelessness was not associated with MRSA in hand infections.85,86 With appropriate support, the majority of PEH were able to complete their course of antibiotics and were not at increased risk for antibiotic failure.87,88 Five studies found that homelessness was not associated with increased mortality.38,42,45,56,57
Educational initiatives
Two studies reported educational initiatives for surgical residents regarding PEH. Freimane and colleagues89 described a virtual conference that included teaching on homelessness and pregnancy. After the conference, there was a reported 78.2% increase in self-assessed “very good” or “excellent” knowledge on homelessness and pregnancy among the participants.89 Lupicki and colleagues90 described a community tour for residents that included a homeless shelter, and after the intervention a significantly larger percentage of participants reported feeling highly prepared to work with impoverished patients. However, less than 13.3% of residents who participated were in surgical specialties.90 Both of these studies were published only as abstracts at the time of our review. A primary study by Sayal and colleagues91 explored the attitudes of medical students and ophthalmology residents working with PEH. Residents had more negative attitudes, less interest, and less confidence working with PEH than medical students.91
Barriers/challenges
Many studies discussed barriers or challenges PEH face when it comes to surgical care, including 48 primary studies,19,31,34–36,39–41,43–45,47–50,54,55,57–64,66,69,72,73,75,79–81,86,91,96, 98,100,102–105,107–109,111,112,114,116 9 abstracts,37,38,42,52,77,84,101,106,118 5 literature reviews,22,74,95,99,110 1 invited article,51 1 magazine article,70 1 thought piece,92 1 ethical essay,115 1 thesis, 71 and 1 historical analysis.117 The majority of comments presented concerns regarding living conditions. The lack of stable housing was described as a possible reason for leaving against medical advice,57 readmission, 54,92 extended hospital stay,55,58,67,87,93,94 and missing follow-up appointments.36,64,79,95–97 In addition, authors commented on how the lack of a regular address leaves home nursing services inaccessible,97 terminal care impossible,49 and deters patients from procedures. 80,98 Furthermore, the need to find shelter and food can come as a priority over pursuing health care.22,43,48,50,59,60,71,98,99 Food insecurity can also pose difficulties in following postoperative diets.84,97 Limited access to transportation prevents obtaining both initial and follow-up care.36,41,50,59,70,71,77,97,100
The living conditions of PEH were described as unsafe43,69,71,97,98,101 and unhygienic36,92,95,97 places to recover after surgery. Prior to surgery, being homeless can contribute to surgical admission; e.g., through an increased risk of traumatic injury due to violence,95 cold exposure leading to frostbite,102 and burns from fire hazards.58 In Canada and other countries that use health cards, living in shelters or on the streets puts people at risk of losing their health cards or having them stolen.99
Higher rates of mental health or psychiatric conditions, including substance use and other comorbidities, can present as a challenge in all phases of surgical care.22,38–40,43,45,51,57,58,63,70,79,86,95–97,100,103–106 PEH can present with more progressed disease and serious conditions affecting indications for and outcomes of surgery.36,43,44,58,60,61,81,92,100,106,107 Treatment compliance following surgery was also documented as a challenge.35,48,103
Systematic barriers within the health care system can impact PEH receiving surgical care39 and lengthen their time in hospital.19,69 Studies commented on how PEH can have difficulty accessing medical care, resulting in fragmented or atypical health care utilization. 22,43,49,51,59,73,74,84,100,108–110 Specifically, 11 studies commented on challenges for PEH accessing specialty care.36,41,43,60,75,92,99,100,103,111,112 Four studies mentioned their overreliance on visits to the emergency department. 41,75,95,103 Two studies commented on how a hospital’s limited funding, resources, space, and personnel can prevent PEH from receiving the care they need while admitted,30,47 and 1 study commented on how PEH can experience more discharge concerns.113 Lack of insurance was noted frequently, even in countries with public coverage but missed certain services.57,59,72,77,99
Thirteen studies mentioned how negative experiences with physicians and other health care providers can be a barrier to PEH obtaining surgical care. Physicians may view homelessness as a contraindication for certain procedures.39,42,66 They may also fail to screen PEH for conditions like colon cancer31,52 or social needs.47 Stigma against PEH can lead to discrimination and power imbalance in decision making.59,80,100,114,115 Overall, PEH can have negative interactions with the health care system that lead to mistrust.38,50,70,91,92,115 Additionally, studies commented on how the perceptions of PEH concerning social pressure in clinics,41 embarrassment with procedures,51,80 inability to pay,70,72 and necessity of the operation39 can act as barriers.
Other factors contributing to the vulnerability of PEH were documented as additional challenges. These included marital status,73 race and ethnicity,73 residential history,73 incarceration,95 language,116 immigration,116 gender,77 and education.50,99 In particular, low income/poverty was the most reported contributing factor, with comments in 13 papers.37,43,45,48,51,58,59,72,73,79,98–100 Lack of social support was also mentioned frequently, with comments in 8 articles.34,36,50,71,79,96–98 Finally, the 2 historical articles highlighted the potential for PEH to be abused for research.117,118
Interventions and future strategies
A few articles were thought pieces aimed at addressing these barriers and challenges. From these articles, suggested future strategies were collected (Box 1). Four articles also described interventions specifically designed to provide better surgical care to PEH (Table 6).
Summary of interventions and their outcomes
Future strategies suggested in included articles
Trauma-informed care and sensitively stewarding informed consent
Development of supportive housing/respite facilities
Routine screening for social determinants of health
Multidisciplinary clinics
Adjustment of care (e.g., alternative operative methods, prolonged period of immobilization and non-weight-bearing for PEH with ankle fracture fixation)
Psychosocial after-care program focusing on anxiety, legal concerns, and depression
Contributing to research on surgical outcomes for PEH
Engaging with local social safety nets by donating surgical supplies and services
Improving medical education and continuing professional development on identifying and caring for PEH
PEH = people experiencing homelessness.
Discussion
This scoping review identified 104 papers describing how PEH interact with surgical care. Homelessness is a complex social issue that reduces access to medical care and further exacerbates barriers within it.11–18 As the scope of this paper indicates, every surgical specialty provides care for PEH. It is important for surgeons to understand how to care for PEH, especially with the rates of homelessness increasing postpandemic.9,10
We chose to broadly investigate the literature surrounding surgical care and PEH. Expanding on the study by Abel and colleagues,22 we included studies performed around the globe, investigated grey literature, and had an enlarged definition of surgical care that advanced past procedures done under anesthesia. The studies included in our review were mainly descriptive in nature. Most studies investigated whether there was an association between homelessness and a specific condition that required surgical intervention. The second-largest type of study was those available only as abstracts, demonstrating difficulty in completing or disseminating this type of research. There were also few qualitative studies identified. As qualitative research seeks to incorporate patients’ voices and perspectives into scientific literature, it can be a useful tool to bring marginalized voices to the forefront of discussion.119
Interestingly, the specialties included within this review matched the distribution of surgical needs of PEH. The study by Zuccaro and colleagues35 was the only one to investigate how PEH interact with different surgical specialties, albeit without the inclusion of ophthalmology, oral surgery, and obstetrics and gynecology. The most frequently contacted services for emergency department referral were orthopedic surgery and plastic surgery. This matched the spread of literature, with most articles referring to those specialties. It is possible that the degree to which a specialty interacts with PEH is being reflected within the literature. However, the study by Zuccaro and colleagues35 was conducted specifically in Ottawa, Canada, and may not reflect the surgical needs of PEH in other parts of the world.
The experience of homelessness is complex and multifactorial, and the circumstances vary from individual to individual. PEH can be found along a spectrum of temporary housing instability owing to life circumstances such as fleeing from domestic violence to chronically sheltering in places unfit for human habitation. When the term homelessness is used, the common understanding is of individuals experiencing housing instability and/or on the lower socioeconomic spectrum. Hence, it was not unexpected that many studies included in our review did not formally define homelessness prior to using the term or describing their study population. When study authors tried to formally define the conditions that qualified as housing instability, the task became increasingly complex as individual authors used varying criteria to capture invisible homelessness through the use of time (e.g., length of stay in a homeless shelter per calendar year) or appropriateness of shelter (e.g., staying with friends). Other circumstances leading to homelessness, such as disaster evacuation and refugee status, can be placed on the spectrum of homelessness but were excluded from our review. Both scenarios were deemed to be outside of the scope of this research. Finally, homelessness is considered to be a transient state; Bennett and colleagues66 continued follow-up of their patients, and 73% of their study population found housing at some point in their postoperative period, demonstrating that homelessness can be transient and not necessarily chronic.
It is also worthwhile to discuss the differences in health insurance around the world, which can be a determining factor in whether a costly surgical procedure or intervention is available to patients. For example, American patients with government insurance or without insurance had lower odds of receiving breast reconstruction postmastectomy in comparison to those with private insurance.120 Even in countries with universal health care, there are medical and surgical options that are not covered by public insurance. Ramsay and colleagues121 described how affordability acts as a barrier for PEH to adhere to physician advice. Given that various aspects of surgical care involve choosing treatments with different costs, it prompts a reflection on the equity of care distribution.
Medical education around PEH is another area of concern. The single study that explored students’ and residents’ perceptions of working with PEH determined that attitudes appeared to become more negative as trainees progressed through training.91 The teaching surrounding working with PEH has been called into question for reinforcing stereotypes and lacking applicability.122 However, although only available in the form of abstracts, the studies that investigated educational initiatives found positive responses among the learners involved.89,90 As interacting with patients with complex social needs without “quick-fix” solutions can be emotionally draining for medical professionals and learners, more interventions to properly prepare students and professionals should be put in place. This, in turn, has the potential to reduce the negative interactions PEH face when interacting with the medical system for there is a negative association between burnout and empathy.123
Limitations
The strength of this study includes its comprehensive approach to the literature search. Our search strategy involved multiple databases, grey literature, and forward snowballing. We also used a definition of surgical care that included all procedures, referrals, and consultations that surgeons may see, as not all surgical care involves the operating room or use of anesthesia. Although a major strength of this study, the broad approach to the topic also acted as a limitation. Owing to the broad search terms used and the general focus on surgery, we cannot claim to have comprehensively reviewed the literature available within each surgical specialty as we did not use specialty-specific search terms. Additionally, as homelessness is a complex experience on the spectrum from transient to chronic, the use of the definition of homelessness varied among articles. It is possible that those experiencing chronic homelessness compared to a brief period of homelessness may have different surgical needs, and it is unclear which populations were included within this review.
Another limitation of this study is the concept of unconscious or implicit bias, in which existing data are informed by ascribing stereotypical characteristics to certain groups without realization.124 For example, PEH being reported as more likely to leave against medical advice and being over-represented in traumatic injuries can contribute to a negative perception of PEH.19–21,38,45,72 Data suggest the phenomenon of negative counter-transference in caring for PEH can develop as early as during training.124,125 If left unchecked, negative stereotypes, bias, and perceptions can affect patient care, research, and advocacy efforts for this population. Thus, action must be taken to educate clinicians and researchers on implicit bias and counter-transference, and tools to address these are needed to reduce the impact on future research, perceptions of the interaction between surgical care and PEH, and consequently the health outcomes of PEH.
Conclusion
This scoping review captured a broad array of literature examining the surgical care of PEH. It identified studies within all surgical specialties. Although PEH often present with advanced medical conditions or traumatic injuries that require surgical operation or management, their access to such care can be limited by various barriers and challenges. Future research stratifying and comparing different health care systems, elective compared with nonelective procedures among PEH, cost-analysis projects, and surveys of the opinions of providers and PEH can provide valuable insight to this topic.
Acknowledgement
The authors thank Sadaf Ullah, clinical outreach librarian at McMaster University, for her assistance with search development.
Footnotes
This work has been presented at the 2023 Bethune Round Table in Global Surgery as a poster presentation, the 2023 AWS Canadian Regional Conference as a virtual presentation, and the 2022 McMaster Global Health Conference: Reimagining Global Health Toward Sustainability and Equity as a poster presentation.
Competing interests: None declared.
Contributors: C. Hircock, P. Huan, and M. McDonald designed the study. C. Pizzola acquired the data, which all authors analyzed. All authors wrote and reviewed the article and approved the final version for publication.
Funding: M. McDonald is supported through a Global Surgery Scholar Bursary awarded by the McMaster University Global Health Office and Departments of Obstetrics & Gynecology, Anesthesia, and Surgery (MacGlObAS).
- Accepted November 9, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/