Abstract
Background: As the population of older adults expands, it is becoming increasingly crucial to develop perioperative protocols to meet their physiologic, functional, and cognitive demands after emergency surgery. We sought to identify protocols that improve the disposition, length of stay, and overall health outcomes of older adults undergoing emergency intracavitary, noncardiac surgery.
Methods: Embase, Cochrane, and MEDLINE databases were searched, and results were deduplicated and uploaded to Covidence. We reviewed studies for postoperative interventions that reduced delirium, maintained functional status, and reduced length of stay in older patients undergoing emergency surgery. We included studies involving patients aged 65 years and older undergoing emergency intracavitary, noncardiac surgeries. Abstracts and full texts were reviewed by 2 reviewers. Data were extracted on the postoperative interventions used and the resulting patient outcomes.
Results: We included 6 studies, which involved patients undergoing emergency general, urology, and vascular surgery. Interventions included a multidisciplinary approach, early involvement of a geriatrician or hospitalist, targeted geriatric-led ward rounds, unique postoperative order sets, and volunteer-driven activities. Standard care included early removal of lines, early mobility, optimal hydration, and medication review. These interventions were associated with decreased length of stay, decreased postoperative complications, and increased likelihood of disposition to home and previous functional status. Frailty was correlated with worse outcomes.
Conclusion: Through multidisciplinary interventions, a successful postoperative protocol for older patients undergoing emergency surgery is helpful for improving patient outcomes. The implications of these findings will help guide our own quality-improvement initiative to improve these outcomes in this patient population at our institution.
As our population of older adults expands, health care professionals are finding it necessary to develop standardized, perioperative management protocols to meet the physiologic, functional, and cognitive demands specific to this population. The popularity of this topic is growing as older patients are undergoing more invasive surgical procedures for cure or rescue.1
Surgeons are no longer avoiding operating on the older patient, which emphasizes the role for perioperative, evidenced-based guidelines. The American College of Surgeons (ACS) Geriatric Surgery Verification program2 and the Coalition for Quality in Geriatric Surgery’s Hospital Standards to Promote Surgical Care of the Older Adult3 are quality-improvement initiatives that provide evidence-based and expert-driven perioperative recommendations to improve surgical care and outcomes for older adults in the elective setting. Alternatively, the ACS Emergency General Surgery Verification Program defines surgical standards for emergency surgery patients with some recommendations for the older patient.4 Areas of overlapping focus include identifying the frail patient, implementing a geriatric expertise service, managing delirium and dementia, establishing patient preferences and goals of care, managing medications, and promoting patient mobility and safe patient disposition. A key difference between emergency and elective surgical patients is the challenge with preoperative optimization for patients undergoing emergency general surgery. These patients ultimately rely on targeted postoperative care to see improvements in length of stay, return to premorbid functional status, and overall health outcomes.
The use of older adult–focused perioperative protocols involving pre- and postoperative comprehensive geriatric assessments and collaboration with allied health professionals has reduced length of stay and other relevant outcomes in the older patient in the elective setting.5 However, these resources for the older patient in the emergency setting have limitations, which creates challenges when developing a standardized protocol.
In this scoping review, we sought to identify postoperative protocols in the literature designed to improve the health outcomes of patients aged 65 years and older after emergency intracavitary, noncardiac surgery. A scoping review was appropriate, as our objective was to explore any evidence in this area, identify relevant themes, and highlight gaps that could be further researched either through focused systematic reviews or targeted prospective cohort studies. This evidence can inform institutions on how to optimize the care of their older adult population after emergency surgery and identify challenges with standardizing emergency, postoperative care in this vulnerable population. Our research question was, What are the postoperative interventions in the literature for patients aged 65 years and older after emergency intracavitary, noncardiac surgery that aim to improve patient health outcomes, patient recovery, and patient return to prehospital functioning?
Methods
We report this scoping review in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR) Checklist recommendations along with updated scoping review methodologic guidance informed by JBI.6,7 The completed PRISMA-ScR checklist can be found in Appendix 1, available at www.canjsurg.ca/lookup/doi/10.1503/cjs.007822/tab-related-content). The protocol is registered with Open Science Framework. Literature searches of Embase, Cochrane, and MEDLINE were performed to identify existing postoperative protocols designed to improve return to preoperative functional status and reduce postoperative complications in the older adult undergoing emergency intracavitary, noncardiac surgery from inception to Sept. 21, 2021. Medical Subject Heading terms included “Aged,” “Elderly,” “Postoperative care,” “Enhanced recovery after surgery,” “Post-Op,” “Emergencies,” “Practice guidelines,” “Quality Improvement,” “Total Quality Management,” “Quality assurance,” and “Protocol.” Results were deduplicated and uploaded to Covidence.8 Details regarding our search strategy can be found in Appendix 1.
Eligibility criteria
Studies were included if they involved patients aged 65 years and older who were admitted for emergency intracavitary, noncardiac surgical care. This included both operative and nonoperative admissions. The specialties identified and included were urology, vascular surgery, and general surgery. The studies must have also included descriptions of pharmacologic, nonpharmacologic, or multidisciplinary interventions used as part of a postoperative protocol. We did not select studies on the basis of outcomes measured because of heterogeneity across studies. Outcomes identified included incidence of postoperative delirium and complications, length of stay, surrogates for functional status and quality of life, or disposition. Study designs focused on quality improvement, before–after, prospective quasiexperimental or cohort, and randomized controlled trials. Studies must have been published in English.
We excluded review articles, meta-analyses, studies based on preadmission interventions, studies of elective surgery, and studies involving patients younger than 65 years or those that did not stratify and analyze by age group when all ages were included. However, review articles were checked for relevant references to be considered for inclusion.
Data extraction and synthesis
Two independent assessors (B.G. and A.N.) reviewed the title and abstracts of retrieved publications based on inclusion and exclusion criteria outlined above. Disparities were discussed among assessors until an agreement was reached. Full texts were subsequently reviewed by the same assessors (B.G. and A.N.). References from included studies and review papers were also reviewed for relevant sources that met inclusion criteria. Through this method, we found 4 additional studies. From full-text publications, we extracted information on design, patient population, outcomes measured, description of the intervention, results, and conclusions. Finally, we implemented the Grading of Recommendations, Assessment, Development and Evaluation (GRADE) method of quality analysis to establish the overall quality of each study.9–11
Results
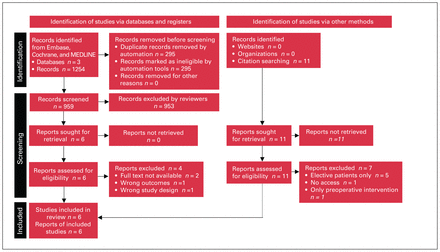
The literature search identified 6 studies that met our inclusion criteria (Figure 1 and Table 1). Results are presented as a narrative synthesis organized first by interventions followed by outcomes. Overall, the outcomes measured either improved or remained unchanged after protocol implementation. Interventions were mostly consistent across studies, with some minor differences.
PRISMA flowchart for study selection.
Summary of included studies
Interventions
The common interventions noted across the studies were multidisciplinary meetings, early involvement of geriatricians or hospitals, standardized admission order sets, patient-centred programs, and formal assessment of frailty.
Multidisciplinary meetings
A multidisciplinary approach was highlighted across the studies. Braude and colleagues,12 Mudge and colleagues,16 and Bakker and colleagues14 used weekly multidisciplinary meetings to allow for dynamic patient care and address any current or anticipated issues with patients. This was also an opportunity for staff members to raise any concerns, both from a patient and intervention perspective. Braude and colleagues implemented targeted geriatric-led ward rounds allowing for further, more targeted interventions, and more frequent progress reports.12 In 2 studies, formal multidisciplinary panels were created to help identify issues and develop a standardized pathway.12,15 The panels consisted of surgeons, hospitalists, nurses, social workers, physiotherapists, and occupational therapists.
Early involvement of geriatricians or hospitalists
Early involvement of a hospitalist or geriatrician was consistent across the studies. Engelhardt and colleagues15 involved a hospitalist to address complex medical conditions and palliative care specialists, should the patient meet a predetermined set of criteria. Khadaroo and colleagues17 used a geriatric assessment team who would assess the patient within 48 hours of admission as per their unique postoperative order set. Bakker and colleagues14 and Koebrugge and colleagues13 would screen patients for frailty and involve a geriatrician if the patient screened positively for “frail” or “delirious.” This would then lead to a series of interventions through the CareWell in Hospital program14 or the high-standard delirium care protocol,13 respectively. Mudge and colleagues16 involved a senior medical practitioner to review patients and co-manage with other services.
Standardized admission order sets
Two of 6 studies created a targeted admission order set.15,17 These order sets standardized postadmission care and helped providers in avoiding treatments that can contribute to confusion and delirium. Most of these interventions are already well established in the elective setting.18 Engelhardt and colleagues15 developed a targeted discharge plan based on conversations with patients and their families regarding expected and realistic length of stay. They also had a multitiered frailty follow-up protocol in which the patients would be phoned at specific intervals after discharge to assess recovery and progress.15 The standardized order set used by Khadaroo and colleagues17 had “intentional comfort rounding,” which is an assessment by nursing every 2 hours in terms of positioning, mobility, hydration, nutrition, pain control, and delirium prevention. The order set also included medication review, and patient and family education.17
Patient-centred programs
Bakker and colleagues14 and Mudge and colleagues16 tasked volunteers to provide cognitively stimulating interventions to the patients, such as puzzles and games. Khadaroo and colleagues17 integrated their BE-FIT (Bedside Reconditioning for Functional Improvements) program, which is a self-administered exercise program patients perform postoperatively to improve recovery, reduce delirium, and return to baseline. Bakker and colleagues14 implemented the CareWell in Hospital program designed to improve patient-centred care for older patients and to educate health care professionals about providing care to older adults. This program also had trained volunteers offer activities for cognitive and physical stimulation to patients, with a goal to prevent perioperative complications, including hospital-associated delirium and functional decline.14
Formal frailty assessment
Frailty was specifically addressed by Engelhardt and colleagues15 and Bakker and colleagues.14 Engelhardt and colleagues used frailty indices validated for both emergency general19 and trauma surgery patients.20 For 3 months, they prospectively screened for frailty in patients older than 65 years admitted for emergency general surgery, and subsequently, those who screened positive underwent the intervention.15 In the study by Bakker and colleagues, through the CareWell program,14 nurses would subjectively complete their own frailty screening based on 6 delirium risk factors — cognitive impairment, sleep deprivation, immobility, vision impairment, hearing impairment, and dehydration — followed by a more in-depth screening by the geriatric nurse.21
Loss of independence
In 4 of 6 studies, loss of independence, a surrogate for functional decline, was evaluated in several different ways. These included assessing activities of daily living (ADLs) performance at 3 months postdischarge, caregiver burden, decline in function or mobility, increased care needs at home, discharge to nonhome destination, discharge to usual residence, and requirement for alternative level of care.14–17
Outcomes
Outcomes measured were variable across studies and representative of success or failure of the entire protocol. Two studies divided outcomes into primary and secondary.14,16 Below are the outcomes identified and the corresponding changes noted postintervention.
Length of stay
Length of stay was determined in 4 of the 6 studies.12,15–17 All showed an improvement in length of stay, although this finding was not statistically significant in 1 study. Braude and colleagues12 found a significant decrease of 19% (4.9 v. 4.0 d, p = 0.01). Khadaroo and colleagues17 noted a significant decrease of a median of 3 days (10 v. 7 d, p = 0.001), and Mudge and colleagues16 found a significant decrease of 2 days (12.6 v. 9.3 d, p = 0.02). In the study by Engelhardt and colleagues,15 the improvement was not statistically significant; the authors noted a length of stay decrease from 9 to 6 days (p = 0.4).
Postoperative complications and surgery cancellations
Two of 6 studies compared postoperative complications, and both found significant decreases (range 19%–24%, p < 0.001).12,17 Braude and colleagues12 also noted fewer cancellations in surgeries due to medical issues, but this was not significant (10% v. 5%, p = 0.12).
Readmission rates, loss of independence, functional decline, and need for alternative level of care
Readmission rates were compared in 4 of 6 studies,12,14,15,17 and overall, these were improved after intervention. However, statistical significance was reached in only 1 study (36.4% v. 10.2%, p = 0.02).15 Loss of independence decreased significantly by 40% (100% to 60%, p = 0.01),15 functional decline was found to improve (39.7% v. 20.6%, p = 0.02),16 and need for alternative level of care decreased significantly by half (39.9% v. 20.7%, p < 0.001).17 Bakker and colleagues14 found a significant improvement in physical decline (41% v. 61%, p = 0.008) and ADLs at 3 months (7.9% v. 9.5%, p = 0.035), as well as a subjective decrease in burden of care for caregivers, although this was not significant (3.1% v. 1.9%, p = 0.126). Mudge and colleagues16 also noted an increase in discharge to usual or previous level of care, but this was not significant (54.2% to 67.6%, p = 0.12).
Delirium rates
Four studies evaluated delirium rates after their interventions.13,14,16,17 Koebrugge and colleagues13 found higher delirium rates (59%) in emergency patients as compared with rates in elective surgery described in the literature (29%–39%).22 The authors did not have preintervention values for comparison.13 Bakker and colleagues14 did not identify a difference in delirium pre- and postintervention (13% v. 12%, p = 0.828). Both Mudge and colleagues16 and Khadaroo and colleagues17 saw significant improvements in delirium after their respective interventions (35.6% v. 16.2%, p = 0.01;16 25.5% v. 12.9%, p = 0.00617).
Quality of evidence (GRADE assessment)
Table 2 shows the assessment of the quality of evidence as per GRADE criteria, and Appendix 1 shows the quality analysis per study.11 Overall, the studies are of low quality owing to their observational nature, indirectness of evidence, reporting and observer bias, and inability to control for confounders. There is no way to determine causality given the lack of randomization and the implementation of multiple, concurrent changes. Observer and reporting bias is also present, as health care workers knew the changes being implemented were to improve these outcomes. Additionally, all patients meeting the criteria were enrolled in the study with no control group. Comparisons were made retrospectively to a smaller pre-implementation group.
Summary of quality of evidence as per GRADE criteria
Discussion
Efforts to improve care for hospitalized older patients undergoing emergency surgery are still ongoing. Emphasis is placed on tailoring treatment based on geriatric expertise, transitional care, and disposition planning, as well as clear communication between care teams and patients and families. These concepts and the impact they have on a patient’s course in hospital, and physical and functional outcomes are demonstrated in this review.
The multidisciplinary approach is well-established in many areas of health care and was consistent across all studies. Shared decision-making and using individual expertise from a variety of professional backgrounds has been clinically and economically effective both in surgical and medical environments.23 The involvement of geriatricians alongside the multidisciplinary team has also been shown to be helpful.24 A comprehensive geriatric assessment holistically evaluates the older person, including medical history, psychosocial circumstances, and functional status, and uses this information to form a multifaceted care plan to aim for return to prehospital functional status.25 Orthopedic surgery was the first surgical specialty to integrate geriatricians into their care team. A meta-analysis of randomized controlled trials (RCTs) saw an improvement in functional status and increased return to prehospital place of residence after implementing comprehensive geriatric care for patients with hip fractures.26 Geriatric care has also been beneficial for medical patients. A meta-analysis of RCTs compared comprehensive geriatric care with usual care for patients older than 65 years admitted to urgent care and found that patients in geriatric-designated wards who received comprehensive older-adult care were more likely to be living at home at their 12-month follow-up visit and had overall improved patient outcomes.27 It is essential to include this in the care of patients undergoing emergency surgery.
Frailty is increasingly being included as a criterion for geriatric intervention, with many described tools providing objective measurements of functional reserve and identifying patients more prone to adverse outcomes.19,28–32 A systematic review and meta-analysis found that the presence of frailty is accurate in predicting postoperative mortality, complications, prolonged length of stay, and loss of independence, with a mortality rate as high as 24.7% among frail patients undergoing emergency abdominal surgery.1 The 2019 report put forth by the ACS Geriatric Surgery Verification program recommends preoperative screening for high-risk characteristics as denoted by frailty tools. It further notes that these concerns should be addressed within 48 hours of admission if in the emergent setting.2 By incorporating frailty, we can identify higher-risk patients within an already-vulnerable population, thereby shifting resources and preventing overburdening of geriatricians. This was demonstrated by Engelhardt and colleagues,15 who had hypothesized that prioritizing frail patients requiring emergency general surgery might delay evaluation and care for nonfrail patients needing emergency general surgery, leading to worse outcomes (e.g., length of stay, loss of independence, or readmissions) in that cohort. Instead, they found that outcomes for nonfrail patients did not drastically change even with resources shifted toward the patients screened as higher risk and frail.15 Frailty is likely a better target for interventions in the older adult than age, which is often arbitrary.
Finally, patient-centred short- and long-term outcomes are increasingly being recognized as a standard of quality in emergency surgical care, with loss of independence being one of the most important and clinically meaningful for patients after admission.33 In 2016, Berian and colleagues found loss of independence to be significantly associated with readmission rates and postoperative complications in older surgical patients, and found that it was the strongest factor associated with death after discharge. They identified several risk factors associated with loss of independence, including age older than 75 years, previous fall history, length of stay, or emergency surgery.34 Recently, patient income below national median has also been found to predict loss of independence, and perceived social support was found to be protective against loss of independence.33 Bakker and colleagues14 were the only researchers who evaluated patient-reported outcomes at more than 30 days postdischarge and found improvements in 3-months-postdischarge ADLs and caregiver burden after implementation of their protocol.14 Maintaining pre-existing mobility and function through careful attention to postoperative care needs may also allow for early recognition of limited home resources, which could provide an opportunity to intervene through increasing social supports before discharge, thus reducing loss of independence.
Limitations
There are certain limitations inherent in before–after studies. Given that there are multiple interventions being implemented at once, establishing causality is impossible without randomization and controlling for confounders. Also, the likelihood of potentially unequal and unidentified confounders influencing the impact of the intervention is high and creates issues with generalizability.
As expected, preintervention data collection would stop once an intervention was implemented, resulting in smaller preintervention cohorts and consequently reduced power.14,15 Engelhardt and colleagues found that retrospectively screening for frailty was difficult given that only chart review was available for preintervention data collection. Retrospective frailty screening typically involved in-person interviews and self-reported data alongside electronic medical record documentation, which on its own has inherent variability.15
Given specifics of the centres in question, there is an issue of generalizability. Centres with a geriatric service may already have better preintervention outcomes than centres unfamiliar with geriatric services, which may need a longer study period to account for the learning curve. Even within a single centre, there may be existing practice variations between the individual providers or wards that may influence outcomes.
None of the studies formally report on patient-reported outcomes, which may be more clinically meaningful. Life-saving surgery may not always be the main patient priority if surgical morbidity is high.
Other limitations included the sample size of the individual studies and resulting statistical analysis. Samples tended to be small and even smaller when subgroup analysis was required. This could lead to loss or gain of statistical significance, creating bias and misinterpretation.
Conclusion
Older adults undergoing emergency general surgery is a rapidly growing area in health care. Standardized protocols and the associated patient benefits are well established in the elective setting. Conversely, thorough preoperative risk assessment and pre-habilitation for older patients in the emergency setting is often not possible, creating challenges with postoperative recovery. A standardized protocol with an individualized multidisciplinary approach involving shared decision-making between the patient, their family, and the health care team may help improve outcomes in this patient population.
Availability of data and material
Footnotes
Competing interests: None declared.
Contributors: Brianna Greenberg contributed to the literature search, study design and analysis, and drafting the manuscript. Stephanie Jiang contributed to the GRADE quality assessment and revising the manuscript. Ashlie Nadler contributed to the literature search, study design and analysis, revising the manuscript, and supervising the work. All authors gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Ethics approval: Ethics approval was waived as this is part of a quality improvement initiative.
Protocol registration: Open Science Framework.
Funding: This work was funded by the Sunnybrook Health Sciences Centre Division of General Surgery Academic Enrichment Fund Grant.
- Accepted December 8, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/