Abstract
Background: The Delta Oasis program was launched in New Brunswick in 2006 to offer patients from rural areas who were undergoing breast cancer surgery and their families 1 night of free accommodations and a postoperative consultation with an extramural nurse. We sought to investigate patient experiences with this program.
Methods: This mixed-method retrospective study took place from 2020 to 2022 and compared the preoperative anxiety and quality of recovery of program participants and control patients who were discharged home over 100 km from hospital. We conducted 2 × 2 analysis of variance to evaluate the effects of intervention group and surgery type. We conducted semistructured interviews with intervention participants, which we then thematically analyzed. Two patient partners were engaged during data synthesis to support the interpretation of results.
Results: We included 34 patients who participated in the program and 18 control patients. No statistically significant differences were found between treatment groups in preoperative anxiety and quality of recovery, regardless of surgery type. Thematic analysis of interviews with 17 intervention participants revealed that they were highly satisfied with the program and that the experience helped reduce stress and discomfort related to their surgery.
Interpretation: The Delta Oasis program is a cost-effective alternative to inpatient care after breast cancer surgery and is highly regarded by rural patients; expansion to other regions with the inclusion of additional low-risk surgeries could help address hospital capacity issues. This study contributes to our understanding of the patient experience with the Delta Oasis program and informs the development of similar programs elsewhere.
In recent decades, developed countries have seen a major increase in outpatient surgeries, which allow stable patients to be discharged home on the same day of surgery after a period of observation.1 Outpatient surgery is advantageous for patients as it minimizes their time away from home and reduces patient costs, wait times, and stress. Moreover, ambulatory surgeries profit the health care system by reducing costs for surgical care and increasing overall efficiency.2
Patient hotels are a relatively novel resource embraced by European health care systems to alleviate capacity demands and support outpatient care by reducing unnecessary hospital admissions.3,4 This model blends evidence-based health care and hospitality to provide patients and their supporters a comfortable atmosphere for rehabilitation. The patient hotel concept is more cost-effective than traditional hospital stays and is related to better patient satisfaction and positive patient health outcomes.3
Although currently not as prevalent as in European countries, patient hotels and similar accommodations are gaining popularity in Canada. The Princess Margaret Cancer Centre Lodge in Toronto offers accommodations for out-of-town patients and their families who are undergoing cancer treatment and can manage their own self-care.5 Similarly, a patient hotel specifically designed to accommodate members of Indigenous communities has recently opened in St. John’s. The Lunar Inn offers culturally appropriate accommodations for residents of Newfound-land and Labrador travelling for medical care. The Lunar Inn is operated by First Light, a nonprofit organization serving the Indigenous communities of Newfoundland and Labrador. All patient-related costs are covered by non-insured health benefits for First Nations and Inuit peoples.6
In Saint John, New Brunswick, an innovative partnership was formed between health care and business organizations to support rural patients undergoing breast cancer surgeries. Breast cancer is the most commonly diagnosed cancer among females in Canada.7 The primary treatments for non-metastatic breast cancer are either a mastectomy or lumpectomy.8 Most patients undergoing lumpectomies in North America are discharged the same day of their surgery.9 Patients requiring mastectomies are usually treated as inpatients, but research suggests outpatient mastectomies are a safe and effective alternative, given appropriate patient selection.9
The care model in Saint John supports outpatient lumpectomies and mastectomies for most patients. However, patients who cannot be immediately discharged are typically admitted to hospital. Among other reasons, like complex health needs, patients are admitted if they live in rural areas and would have difficulty accessing emergency medical care in the event of postoperative complications.
Given that 51% of New Brunswick’s population resides in rural communities,10 many patients undergoing breast cancer surgeries must stay in hospital as inpatients, pay out of pocket to stay at a hotel nearby, or travel far distances home upon discharge. Moreover, treatment-related costs are significantly higher for patients with breast cancer than other patients, including spending an average of $225 monthly on necessary travel.11
In response to these hardships, the New Brunswick Breast Health Program and the Delta Brunswick Hotel developed the Delta Oasis program. The program gives patients undergoing breast surgeries who would need to be admitted as inpatients for geographic reasons 1 night of free accommodations, including complimentary meals, valet parking, and extramural care. The Delta Brunswick provides a quiet environment in which patients can recover and is within proximity of both major city hospitals. Eligible patients are identified by a nurse navigator based on the patient’s discharge disposition and proximity to their surgical treatment centre (> 100 km away). We sought to investigate patient experiences with this program.
Methods
We conducted a mixed-methods evaluation to investigate patients’ experience with the Delta Oasis program from 2015 to 2020. Using surveys, we quantitatively evaluated the effects of the program on patients’ preoperative anxiety and recovery quality. Furthermore, we explored patients’ satisfaction with the program and its impact on their perceptions of the Delta Brunswick. Semistructured interviews garnered a more in-depth understanding of patients’ experiences with the program and breast cancer surgery. We engaged patient partners during the data synthesis phase of this project. They contributed to the interpretation of the results and offered their perspectives based on their lived experiences with breast cancer.
Participants included a retrospective sample of patients who underwent an outpatient lumpectomy or mastectomy from 2015 to 2020 at the Saint John Regional Hospital and used the Delta Oasis program. We also recruited a control group of patients who underwent these surgeries at The Moncton Hospital and were discharged to a home more than 100 km away.
A nurse navigator called eligible participants to explain the purpose and nature of the study and request their voluntary participation. Interested individuals were emailed a link to Opinio, an online survey platform, to provide their informed consent and complete a closed survey. Survey recruitment began in August 2020 and ended in October 2021.
Measures
We developed a study-specific questionnaire to collect participants’ demographic characteristics, as well as diagnosis and treatment history.
We used the Preoperative Anxiety Visual Analog Scale (VAS)12,13 to assess participants’ preoperative anxiety. The scale contains 10 items rated on an 11-point scale ranging from no anxiety to extreme anxiety. The validity of the scale was established in previous research involving patients with breast cancer and the internal reliability in the present study was good (α = 0.89).
We evaluated participants’ recovery using the Post-operative Quality of Recovery Scale (QoR-15),14 which measures patients’ health status after surgery and anesthesia. The scale consists of 15 items measuring pain, physical comfort, physical independence, psychological support, and emotional state after surgery. Items are rated on an 11-point scale ranging from none of the time to all of the time. The internal reliability of the scale was good (α = 0.87).
We developed an 18-item study-specific questionnaire to assess the participants’ satisfaction with the Delta Oasis program and their perceptions of the hotel.
Data collection
Participants completed the demographic questionnaire first, followed by the VAS and QoR-15. Finally, Delta Oasis participants completed the questionnaire about their program experiences. Participants could review and change their answers during the survey. Data were stored on the Opinio platform until data collection was complete; data were then downloaded onto the secure computers of research team members and imported to SPSS for analysis.
Participants who used the Delta Oasis program were asked to indicate their interest in participating in an interview to further describe their experiences. A research team member who was previously unknown to the participant called interested individuals to explain the purpose and nature of the study and their role in the project. If the participant was still agreeable to participate, the team member scheduled a semi-structured telephone interview at their convenience.
A female clinical research assistant with a graduate education (S.B.) and qualitative research training, conducted the interviews over the phone, following an interview guide (Appendix 1, available at canjsurg.ca/lookup/ doi/10.1503/cjs.004923/tab-related-content). The interviews were audio recorded and lasted an average of 24 minutes. A member of the research team transcribed interviews verbatim and then uploaded them to NVIVO, a qualitative analysis software. Interviews were conducted until all interested individuals had an opportunity to participate.
Patient engagement
The results of the quantitative and qualitative analyses were subsequently discussed and interpreted further by 2 patient partners and clinical team members. One of the patient partners resided in Saint John at the time of the study and participated in the Delta Oasis program after their breast cancer surgery. The second patient partner resided in Moncton and travelled to their home once discharged from hospital after breast cancer surgery.
Statistical analysis
We used descriptive statistics to summarize participants’ demographic and clinical characteristics and their experiences with the Delta Oasis program. Furthermore, we conducted 2 × 2 analysis of variance (ANOVA) to evaluate the effects of the intervention group and surgery type on participants’ preoperative anxiety and quality of recovery.
Two members of the research team analyzed interview transcripts using iterative–inductive thematic analysis formulating themes through consensus.15
Ethics approval
All materials and procedures were reviewed and approved by the Horizon Health Network Human Research Protection Program (no. 100884).
Results
Participants
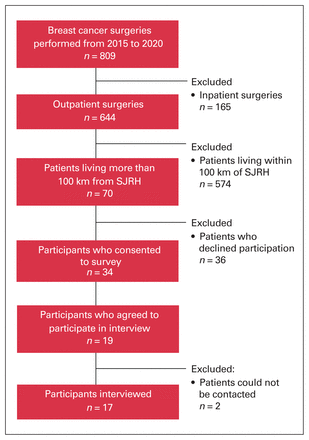
There were 809 breast cancer surgeries performed during the study period (2015–2020); 644 (79.6%) were conducted on an outpatient basis, and 70 (10.9%) of those were for patients who lived rurally, making them eligible for the program (Figure 1). For reference, the Moncton Hospital performed 1003 breast cancer surgeries during the study period, while about 13% of these patients resided rurally.
Study flow chart. SJRH = Saint John Regional Hospital.
Seventy patients who participated in the Delta Oasis program met the study criteria and 34 participated in the study, resulting in a response rate of 48.6%. Sixty-four patients from the Moncton Hospital were contacted about participating in a control group and 18 agreed, leading to a response rate of 28.1%. Demographic and clinical characteristics of the participants are shown in Table 1. Nineteen Delta Oasis participants agreed to be contacted for an interview and 17 participated (2 patients could not be contacted). The interviews were conducted via telephone from January 2021 to August 2021.
Demographic and clinical characteristics of Delta Oasis and comparison groups
Quantitative analysis
All participants except for 1 reported staying at the Delta the night of their surgery; several also stayed the night before surgery. Participants’ quality of sleep varied both nights but was generally fair to good. Most participants also took advantage of the complimentary dinner and breakfast, and all recalled the quality being good or very good. All participants were accompanied by someone at the Delta, typically their spouse or partner. None of the participants reported any health problems during their stay.
All participants (except 1 whose response was missing) indicated that they were likely or very likely to recommend the program to others. Furthermore, most participants indicated that the program increased or greatly increased their likelihood of staying at the Delta Brunswick Hotel and their likelihood of recommending the hotel to others.
All groups of participants reported relatively low levels of preoperative anxiety and high quality of recovery (Table 2). The results of the ANOVAs revealed no significant differences between treatment or surgery groups on preoperative anxiety or quality of recovery (Table 3). Although these results should be interpreted with caution considering the small sample size, the significance of the tests combined with the small effect sizes suggest that the program did not have a meaningful effect on these outcomes, regardless of the type of surgery.
Descriptive statistics of intervention and surgery groups*
Results of 2 × 2 analysis of variance on preoperative anxiety and recovery
Qualitative analysis
Thematic analysis found 7 themes regarding the experiences of participants in using the Delta Oasis program. Exemplar quotations of the themes described in detail below are found in Table 4.
Qualitative analysis themes
The Delta Oasis program was a positive experience
All interviewed participants expressed positive experiences with the Delta Oasis program, stating it was a positive part of their overall care experience. The accommodations, food, and staff were said to be excellent and hugely appreciated. Many interviewees enjoyed having the kitchenette and separate room, so they could sleep while their family member watched television.
Similarly, most participants expressed that the hotel stay was relaxing, provided them a break in their daily routine, reduced some financial burden associated with cancer treatment, and reduced stress. When asked, participants stated that the Delta Oasis program positively influenced how they felt about Delta hotels, indicating that they tell people about the program and make the effort to visit when they are in the city.
Reassuring to have family with them
Most participants found it reassuring to have their family with them at the hospital while they had surgery. They appreciated that the Delta Oasis program provided accommodations and food for them as well, especially after their wait at the hospital. Participants noted that having family members stay with them after surgery provided them with a sense of calm, especially overnight.
Not having to drive home after surgery reduced stress
Participants expressed that knowing they had a place to stay reduced their stress because they did not have to make a long drive home while feeling ill after surgery. Moreover, they expressed concerns about weather; a participant (P5) explained, “I don’t like driving in the winter… so I would have been stressed.”
Reassuring to be close to the hospital
Most participants felt reassured that they would be close to the hospital after their surgery and felt safer about being nearby in case of an emergency. Some participants even mentioned that if they were not able to stay at the Delta, they “would have rather stayed in the hospital because [they were] worried” (P16).
Reassuring to have follow-up care from extramural nurse before going home
Generally, participants felt relief that the program included a next-day visit from an extramural nurse in their room at the Delta. Participants felt the nurse provided compassionate care and were reassured by the clinical visit that they were cleared to make the trip home.
Staying at the Delta had a positive effect on surgery and recovery experiences
When asked, most participants felt that being able to stay at the Delta had a positive effect on how they felt going into surgery. One participant (P6) described that they “just had to be concerned about the day of the surgery.” After surgery, participants expressed that the program positively affected their recovery by allowing them to relax without worry about travel time or being far from the hospital. Participants were pleased that they did not have to stay at the hospital after surgery and instead had a room at the Delta where they could begin their recovery.
Improvements that could be made to the Delta Oasis program
Most participants did not feel there was any way to improve the program specifically, although one did express the need for more communication between hotel staff and another expressed that the program could benefit from offering transportation from the hospital to the hotel for patients who need it. When asked if the Delta Oasis program should be expanded, most participants said they felt it would be beneficial for patients undergoing other types of surgeries, and in other regions in the province and the country. Participants felt that “there’s probably a lot of people that could benefit from [Delta Oasis so] … they don’t have to make that long drive home” (P12). Some interviewees also noted that the program could help with hospital bed shortages by freeing up space for inpatients.
Discussion
We found that participation in the Delta Oasis program had no significant effect on preoperative anxiety and quality of recovery among patients who underwent a mastectomy or lumpectomy. However, interviews revealed that participants who stayed at the Delta were satisfied with the program, and most felt that it reduced their stress and contributed to a positive mindset regarding their surgery and recovery.
Patient hotel models such as the Delta Oasis program are a relatively novel concept and, therefore, their effectiveness is understudied.3 The high satisfaction reported by program participants is consistent with other patient experiences with non-medicalized accommodations after surgery.3,16,17 Compared with traditional hospital stays, patients report greater autonomy, privacy, and feelings of well-being while at a patient hotel.3 In line with previous research, program participants recommend this type of care to others and, given that the Delta is situated near both hospitals in Saint John, participants felt reassured that they would receive necessary care in the event of an emergency.16
Patients who underwent breast cancer surgery appreciated having family members at the hotel after the operation, a notion commonly expressed in related studies.3,17 Likewise, programs such as the Delta Oasis can help reduce the burden of care often felt by patients’ family members. Research has highlighted that family members are comforted knowing their loved one is cared for by both hotel staff and health care professionals.16 The care provided by the Delta to patients and their families is a consideration that is especially pertinent to the well-being of patients undergoing breast surgery who, as females, may themselves feel a responsibility to care for family members upon returning home from the hospital. Previous research has underscored that traditional gender norms may lead women with breast cancer to put the needs of their families above their own health, even when they require care.18 Moreover, those living rurally, like those in the present study, may have more difficulty accessing cancer-related health services. Time spent travelling long distances for appointments and procedures could strain family dynamics since women tend to disproportionately carry the load of care work within the household, even when they are sick.18,19 The Delta Oasis program may relieve some of the caregiving paradoxes faced by many patients with breast cancer, at least temporarily, by giving them the opportunity to focus on self-care.
There are substantial financial implications associated with the Delta Oasis program that could yield health system savings;20 hotel accommodations are 5 times less costly than traditional hospital stays for perioperative care for breast surgery.17 A Canadian study estimated that costs for inpatient hospital stays for breast cancer surgery average around $6600 per patient.21 The Delta Oasis program is a beneficial alternative to inpatient care, which is often not medically necessary for breast cancer surgery. Thanks to the innovative partnership between Saint John’s Breast Health Program and Delta Brunswick Hotel, the Delta Oasis program generates zero cost to the provincial health care system. Establishing funding partners and adapting this service to other types of low-risk surgery could bring forth added health system savings. Participants expressed how beneficial the Delta Oasis program could be for other surgical patients, and research has indeed demonstrated success for patients undergoing low-risk surgeries.16
The research team plans to expand on the current study by conducting a prospective cost–benefit analysis and analysis of the patient experience associated with the Delta Oasis program. In addition, we intend to investigate the potential for expanding the program to include other low-risk surgical cohorts across provincial health zones. Researchers and clinicians who are interested in starting similar programs are encouraged to engage their local surgical units and hotels to determine if a comparable program is feasible.
In New Brunswick, the Indigenous community represents 4% of the total population, with 61% residing in rural communities.22 Living rurally may pose geographic-related health challenges for Indigenous peoples, such as limited access to health services and the burden of travelling long distances to receive care. Inequitable access to care contributes to poor health outcomes such as cancer, which is one of the leading causes of death among Indigenous peoples in Canada;23,24 the rate of cancer is disproportionately higher in Indigenous communities than in non-Indigenous communities.25 Given the complex and fragmented delivery of health care and Indigenous health programs in Canada, cancer treatment and aftercare is especially difficult to navigate for Indigenous patients and their families.26
In a recent needs assessment, Sedgewick and colleagues27 determined that Indigenous-specific accommodations for patients with cancer in Saskatchewan, known as cancer lodges, were underutilized by community members. Patients expressed that this was because of a lack of culturally appropriate care, experiences of racism, and concerns for privacy. Researchers identified a need for greater cultural sensitivity in cancer-related health care and the need to address travel-related barriers such as transportation and accommodations for patients.27 A similar investigation could be conducted in New Brunswick by partnering with Indigenous communities across the province to assess the breast cancer surgery–related needs of outpatients with the goal of implementing culturally supportive accommodations through the Delta Oasis program.
Limitations
Our study’s small sample size is a limitation that could have resulted in the lack of statistical difference in preoperative anxiety and perceived quality of recovery between the Delta Oasis group and control group. Moreover, biases may have affected participants’ responses. Specifically, participants were pleased with the health care they received and experienced uncomplicated recoveries, which could have influenced their perception of the Delta Oasis program. Some participants were surveyed years after their experience with the Delta, which could contribute to recall bias affecting their recollection of preoperative anxiety and quality of recovery.
Conclusion
The Delta Oasis program is a cost-effective alternative to inpatient care after breast cancer surgery and is highly regarded by rural-dwelling patients. Furthermore, expanding the program across other regions with the inclusion of additional low-risk surgeries could help address hospital capacity issues. We used a mixed-methods approach and engaged patient partners to glean a full understanding of the patient experience with the Delta Oasis program and to inform the development of similar programs elsewhere.
Footnotes
This study was presented at the New Brunswick Health Research Foundation 2021 Health Research Week.
Competing interests: Sharon Chiu reports consulting fees from Merck and conference support from Allergan. No other competing interests were declared.
Contributors: Sharon Chiu, Samantha Fowler, Heather Tait, and Lauren McLaughlin contributed to the conception and design of the work. Sarah Bridges, Jordan King, and Sarah Street collected data. All of the authors contributed to data analysis and interpretation. Sharon Chiu, Samantha Fowler, Sarah Bridges, and Adrienne Gulliver drafted the manuscript. All of the authors revised it critically for important intellectual content, gave final approval of the version to be published, and agreed to be accountable for all aspects of the work.
Funding: This was an unfunded study, but some members of the research team (Gulliver, Fowler, McLaughlin, and Bridges) were supported by the Canadian Institutes of Health Research and ResearchNB.
- Accepted December 1, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/