Abstract
Background: Rural general surgeons perform many procedures outside the conventional scope of the specialty. Unique to British Columbia, the Rural Practice Subsidiary Agreement (RSA) formally defines rurality in the province. Our goal is to understand the scope of practice for BC’s rural general surgeons and whether it has been affected over time by changing privileging guidelines.
Methods: Medical Services Plan (MSP) data were collected from 2011 to 2021 for procedures billed by general surgeons in communities defined by the RSA as rural. We categorized codes from the MSP based on surgical specialty. For each community, we calculated the totals for these categories considering what other surgical specialties were present as well as changes over time.
Results: From 2011 to 2021, 222 905 procedures were performed in 23 rural communities in BC. Colonoscopies were the most frequently performed procedure (n = 80 114, 35.9%), followed by colorectal (n = 23 891, 10.7%) and hernia procedures (n = 20 911, 9.4%). The most common unconventional procedures were plastic surgeries (n = 8077, 3.6%). Classification within the RSA did not significantly influence the percentage of unconventional general surgery procedures performed (p = 0.4). When another surgical specialty was present, there was often a decrease in the number of that specialty’s procedures performed by general surgeons. Over the past decade, rural general surgeons performed fewer unconventional general surgery procedures (p < 0.001).
Conclusion: General surgeons working in rural communities perform a variety of procedures based on resources, community need, and access to other specialists. Over the last decade, this appears to have been influenced by new privileging guidelines. Understanding the scope of rural general surgery can inform training opportunities and, as there is a migration away from rural surgeons performing as many unconventional procedures, can elucidate the implications on patients and communities.
For Canadians in rural, remote, and northern settings, access to specialty surgical care is more challenging than in urban communities. Although the Canada Health Act states that its primary objective is “... to facilitate reasonable access to health services without financial or other barriers,” patients living in rural communities face multiple barriers to accessing surgical care.1 These barriers are, in part, due to complex social, political, and geographical factors governing Canada’s vast and diverse rural landscape. To bridge the gap in surgical care, general surgeons in rural communities have been noted to practise a larger breadth of skills to provide access to subspecialty surgical care in these communities.2–5 Consequently, the practice patterns of Canadian general surgeons working in rural settings reflect both the needs of their catchment area and the potential paucity of other surgical specialties serving these communities.2,6–10
Surgical practice in rural and isolated settings provides unique opportunities to exercise clinical problem-solving. Rural general surgeons are poised to overcome unique pressures given that they work with limited resources, potentially working in geographically as well as professionally isolated locations, and they must maintain a broad range of skills and knowledge to treat diverse pathologies. The scope of practice for surgeons working in these communities may vary from the general surgery training requirements prescribed by the Royal College of Physicians and Surgeons of Canada (RCPSC).2,11 Previous studies have shown that general surgeons working in rural communities perform more gynecologic, vascular, urologic, orthopedic, and plastic surgery procedures than their urban counterparts.11–13 In 2015, the College of Physicians and Surgeons of British Columbia adopted a new policy on criteria-based privileging, which aimed to define the scope of practice for all specialties including general surgery.13 The impact of these policies on actual practice patterns is unknown and not well understood.
In the province of British Columbia, the Rural Practice Subsidiary Agreement (RSA) between the Government of British Columbia, Doctors of BC, and the Medical Services Commission provides a formal definition and categorization of rurality in the province.14 This agreement was created to improve access, resource allocation, and support for rural communities and care providers. The definition of rurality in BC is based on access to larger medical centres and other specialists, population, and geography. Other jurisdictions have also used population and proximity to metropolitan areas to define rural health care, as well as availability of specific hospital resources and health authority designations.2,15–18 Statistics Canada has defined rural as areas outside of population areas, which have at least 1000 people and a population density of 400 people or more per square kilometre, but does not take resources and health care providers into consideration.19 Although BC has clearly identified and categorized rurality for provincial health care, there is no universal agreement on what identifies a rural community in the literature.
By having a formal definition of rural and remote locations in BC, we are able to identify providers in these areas and understand their scope of practice. In this study, we sought to understand the landscape and changing face of rural general surgery practice in BC, based on time-based and policy-related changes.
Methods
We performed a retrospective observational study evaluating rural general surgery in BC. Rural communities, as defined by the RSA, were selected for data collection. Data were obtained through the Doctors of BC and the BC Ministry of Health Medical Services Plan (MSP) fee-for-service billing codes. These data are publicly available by request, and no identifiable patient or provider information was included; therefore, no ethics approval was required. Our data request included surgical procedures billed by general surgeons in RSA-defined rural communities between 2011 and 2021, organized by community. Communities that are no longer listed under the RSA rural communities (Kamloops, Chilliwack, and Western Communities) were excluded from analysis.
Information about other specialists working in each community was collected through the Doctors of BC MSP database. We collected data on cardiac surgery, gastroenterology, neurosurgery, obstetrics and gynecology, cardiology, otolaryngology, vascular surgery, and urology for each of the RSA communities from 2011 to 2021. Again, no identifiable patient or provider information was included.
Data stratification
Communities were stratified by the categorization defined in the RSA. These categories are designated A, B, C, or D depending on the number of designated specialties within 70 km, the number of general practitioners within 35 km, community size, distance from a major medical community, degree of latitude, presence of a specialist centre, and location arc (air or flight distance to quaternary centre in Greater Vancouver).
We organized the MSP fee codes into categories of abdominal, breast, skin and soft tissue, orthopedic, obstetric and gynecologic, neurosurgical, vascular, urologic, plastic, head and neck, and thoracic surgeries as well as endoscopy and pacemaker or port placement. Subcategories were then created for each heading.
Statistical analysis
We calculated totals of surgery types for each of these communities, as well as overall. The most common core general surgical procedures and unconventional general surgery procedures were determined. We analyzed trends in procedures performed over time using 2011, 2016, and 2021 fiscal years as t = 0-, 5-, and 10-year points. A χ2 test was completed to determine whether there was a statistical difference in the proportion of procedures performed by general surgeons at these time points. We used 1-way analysis of variance to determine the significant difference between the proportion of nonclassic general surgery cases done in RSA A, B, and C class communities by general surgeons. For each community, we also took into account what other specialties existed in each of these communities to see how this shaped general surgical practice. We completed t tests, assuming unequal variance, to determine whether there was a significant difference in the proportion of other specialties’ procedures done by general surgeons, depending on whether that specialty was based in the same community. Statistical analysis was performed on Python.
Results
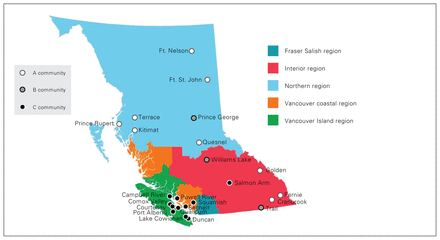
From 2011 to 2021 in BC, 222 905 procedures were performed in 23 RSA-defined rural communities by general surgeons. Of the 23 communities, 7 were in the Northern Health Authority, 7 in the Island Health Authority, 6 in the Interior Health Authority, and 3 in the Vancouver Coastal Health Authority (Figure 1). None were located in the Fraser Health Authority.
Geographic distribution and Rural Practice Subsidiary Agreement rurality index designation of BC communities where a general surgeon was based.
There was a median of 9678 procedures done in each community per year (interquartile range [IQR] 3969– 17 164) and a median of 21 907 total procedures performed in RSA communities each year (IQR 19 911– 24 001). Overall, 90.0% of procedures performed were general surgery procedures, with 10.0% nonclassic general surgery procedures. The most common procedures performed overall were colonoscopies (n = 80 114, 35.9%), followed by colorectal procedures (n = 23 891, 10.7%), then hernia procedures (n = 20911, 9.4%) (Table 1). The most common unconventional procedures performed were plastic surgery (n = 8077, 3.6%), port or pacemaker placement (n = 4145, 1.9%), and vascular surgery (n = 3783, 1.7%) (Table 2). Of the plastic surgery procedures, skin procedures such as flaps or grafts were the most common procedures (n = 4429), followed by procedures on nerves (n = 1853), and hand procedures (n = 1119). For intravascular device insertion, 737 port insertions and 3408 pacemaker surgeries were performed over this 10-year period.
Conventional general surgery procedures performed by general surgeons in rural British Columbia, 2011–2021
Most common unconventional general surgery procedures performed by general surgeons, 2011–2021
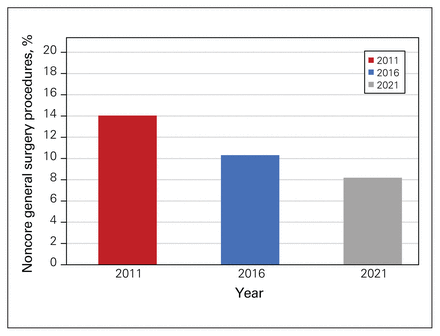
There was a significant difference in the proportion of nonclassic procedures performed over time (p < 0.001). During the 2011/12 fiscal year, 14.0% of procedures were noncore general surgery procedures. At the 5-year mark, 10.3% were noncore general surgery and at 10 years in 2021, 8.2% were noncore general surgery procedures (Figure 2). The overall trend was that general surgeons performed fewer unconventional surgery procedures over time with statistical significance between time points 0 and 5 years (p < 0.001), 5 and 10 years (p < 0.001), and 0 and 10 years (p < 0.001).
Proportion of unconventional procedures being performed by general surgeons in 2011 (t = 0 yr), 2016 (t = 5 yr), and 2021 (t = 10 yr).
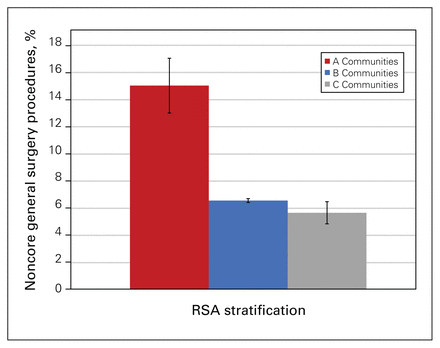
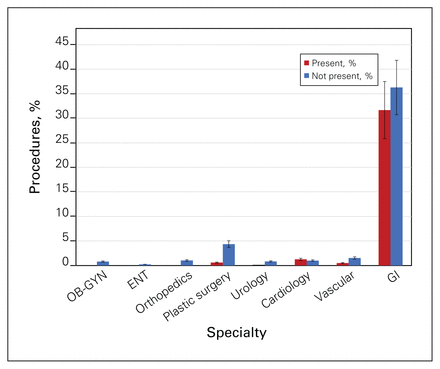
When stratified by RSA classification, there was no significant difference in the percentage of nonclassic general surgery procedures performed (p = 0.4) (Figure 3). There was variable significance in the proportion of other specialty procedures performed by a general surgeon depending on whether that specialty was also based in that RSA community. For communities with an obstetrician–gynecologist, 0.3% of a general surgeon’s case load was in obstetrics and gynecology. In contrast, when there was no obstetrician–gynecologist based in that community, 2.7% of a general surgeon’s practice was in obstetrics and gynecology (p < 0.01). This was also true for orthopedics (0.4% v. 1.8%, p < 0.01), plastic surgery (0.9% v. 5.7%, p < 0.01), urology (0.1% v. 2.0%, p < 0.01), and vascular surgery (0.7% v. 1.9%, p < 0.01). This same theme was not true for ear, nose, and throat (0.4% v. 0.4%, p = 0.5), cardiology (2.0% v. 1.7%, p = 0.6), and gastroenterology (33.4% v. 36.3%, p = 0.4) (Figure 4). Of note, there were 4 RSA communities with both a general surgeon and a gastroenterologist.
Proportion of general surgery versus unconventional general surgery cases performed, stratified by Rural Practice Subsidiary Agreement (RSA) classification.
Proportion of other surgical specialty procedures performed by a general surgeon dependent on presence of that specialty based in the same Rural Practice Subsidiary Agreement (RSA) community. ENT = ear, nose, and throat; GI = gastrointestinal; OB-GYN = obstetrics and gynecology.
Discussion
In our retrospective observational study, we found that general surgeons working in varied rural centres across BC perform a multitude of procedures, including many that are considered outside of the usual realm of general surgery. Our results are similar to those of another Canadian study, which found that the most common surgeries performed by general surgeons are hernia repairs, gall-bladder and biliary procedures, excision of skin tumours, procedures involving the colon and intestines, and mastectomy and other procedures involving the breast.2 This same survey found that colonoscopy followed by esophagogastroduodenoscopy are the most common procedures performed by rural general surgeons.2
In rural BC, 39.9% of rural general surgeons’ practice is endoscopy. At centres with gastroenterology, this becomes 31.7% of a general surgeon’s practice. In rural BC, there are gastroenterologists based in 4 of 23 rural communities where there is also a general surgeon. Similar studies performed in Canada show that endoscopy is the most common procedure, at 51% of all procedures performed by rural general surgeons.2,12 Similar results have been seen in the United States and Australia, with endoscopy making up 24%–52% of rural general surgeons’ practice.4,6,7,20–22 Surgeons and residents interested in rural community practice may seek enhanced training and exposure to high-quality endoscopy, including therapeutic interventions. Proposals to improve endoscopy training during residency include synoptic reporting about quality measures, enhanced skill courses, and partnerships with gastroenterology to increase exposure to emergency and therapeutic procedures.23
We found that 10.0% of BC’s rural general surgeons’ practice falls outside of conventional core competencies. Despite the varied procedures being performed by rural general surgeons, there was a significant decrease in the proportion of unconventional general surgery procedures performed between 2011 to 2021. This is also reflected by a migration toward general surgery subspecialization, with more residents pursuing fellowship and graduate degrees.2,24 Up to 70%–80% of general surgery residents are now pursuing fellowship training and, with general surgery training often being focused in urban centres, there can be a lack of exposure to the clinical scope of rural and community general surgeons in training.25 Furthermore, there is a decrease in the number of “off-service” or non–general surgery rotations being done throughout residency. At the University of British Columbia, general surgery residents complete one 4-week block of gastroenterology in their first year and two 4-week blocks dedicated to endoscopy in third year. Otherwise, they do not spend time on other subspecialty surgical or medical services. Historically, residents completed mandatory rotations in vascular surgery, psychiatry, and emergency medicine. With this said, there is a decrease in exposure to these procedures and skills that would be introduced by completing off-service rotations that may be useful for broad-scope community practice and subspecialty practice, such as trauma surgery.
The proportion of noncore general surgery procedures done in rural BC is lower than in previously cited literature.2,12 This may be partly due to the growing number of general practitioners with enhanced surgical skills (GP-ESS) in Western Canada.26 These practitioners perform common procedures in communities without access to general surgery, obstetrics, and urology. These procedures include herniorrhaphy, appendectomy, endoscopy, management of perianal disease, cesarean delivery, management of labour and delivery, dilation and curettage, skin flap surgery, amputation, vasectomy, tubal ligation, circumcision, tonsillectomy, and carpal tunnel release.27 This wide scope of practice has been found to be controversial given a standardized 1-year enhanced training program but has helped increase access to surgical care for people in rural areas.28
Plastic surgery, pacemakers, and port placement, as well as vascular procedures, have been found to be the most common nontraditional general surgery procedures performed by general surgeons in BC. In a 2020 multicentre study, Schroeder and colleagues found that procedures that are not listed in the RCPSC training objectives but were regularly performed by rural general surgeons included pacemaker insertions, vasectomies, cesarean deliveries, tonsillectomies, fracture management, and female sterilization.2 There have been consistent findings in studies performed in the US.3,4,10 Specifically, a scoping review in 2021 showed that 20.7% of procedures performed by rural surgeons are noncore general surgery procedures.3 Of these, 10.6% were obstetrics procedures, 5.7% orthopedics, 3.2% urology, 3.2% vascular, 1.7% otolaryngology, 0.5% neurosurgery, and 0.1% ophthalmology.3 Suggested procedures for graduating residents to be competent in before entering rural practice include plastic surgery (carpal tunnel repair, ganglion excision, flaps), urology (orchiectomy, testicular torsion surgery), obstetrics and gynecology (oophorectomy, salpingectomy), otolaryngology (thyroid surgery, tracheostomy), and neurosurgery procedures (burr hole, craniotomy).12 This was echoed in other studies also identifying gaps in training for external fixation for fracture management, uterine hemorrhage management, cesarean delivery, nephrectomy, and circumcision.3
In Canada, about 10% of general surgeons work in a rural setting, but most residency programs are based in urban hospitals, often with limited exposure to nonurban centres.2 Suggestions have been made for early exposure to rural general surgery so that residents will later be able to tailor their training toward this.29,30 Furthermore, rural-based fellowships or related training programs to obtain enhanced skills have been proposed for those interested in rural surgery.12 Critiques of enhanced-skills training programs argue that this can become a barrier for residents to enter rural practice owing to the time commitment of additional training as well as resident preparedness for a broad-based practice by the time of graduation from residency.31 Careful succession planning and peer teaching may allow for incoming staff to obtain enhanced skills that historically have been provided in specific rural surgical practices and to support the transition of surgical providers.12
Rural hospital care teams are reliant on each other in different ways compared with urban centres. The practice patterns of rural general surgeons is influenced by the presence of not only other surgical specialists, but also radiology, family medicine, and anesthesia.32–34 For example, patients living in rural communities sometimes must travel to larger centres for radiology-based procedures, such as core biopsies.35 In these situations, not only does the patient have to travel long distances from home for their procedure, but the local rural surgeon may also lose that patient to urban centres. Losing elective work at smaller sites has implications over the long term for rural patients’ access to a surgeon in a timely manner, as a baseline volume of elective work is required to maintain delivery of care, such as cesarean deliveries.36 Furthermore, the BC privileging dictionary, which defines scope of practice in BC, limits general practitioners with enhanced training in anesthesia in elective situations, but not in emergency situations.37 The BC privileging dictionary also has clauses regarding enhanced training and surgical volumes for general surgeons to provide care beyond the classic scope of the specialty.38 This may have a negative impact on new practitioners facing barriers in incorporating nontraditional procedures in their skill set, thus adding to the challenges to accessing care for rural patients. Therefore, besides adequate surgical training, supporting elective practice and policies that incorporate rural patient care concerns are key to keeping specialists and surgical services available to the rural population closer to home.
Currently, the University of British Columbia has the only general surgery training program in the province. General surgery residents at the university have the opportunity to spend up to 24 months in community settings and have the opportunity during senior years to complete 3–6 months of non–general surgery electives. In a 2019 American survey of rural general surgeons, respondents felt “well prepared” (mean of 4.8 on a 1–5 Likert scale) for rural practice after residency. However, a 2021 survey found that only 3% of BC’s surgeons believe recent general surgery graduates are “definitely prepared” for a broad-based community practice, with 49% stating that graduates are “probably not” or “definitely not” prepared.12 Inherent to rural surgery is a degree of professional isolation and the need to manage a wide variety of pathologies.39 Therefore, bolstering resident confidence in working independently and problem-solving is imperative for preparing them for rural practice.
Having general surgeons trained to provide a variety of procedures in rural, isolated, or Northern settings has a great impact on communities. For example, when local surgical services were available, 47% of women were able to deliver locally compared with only 15% when local cesarean delivery services were not available.36 Patients have been shown to prioritize receiving surgical care closer to home for not only their social supports and ease of transportation, but also the community and shared cultural understanding between the patient and health care providers.40 Patients have expressed the importance of familiarity with the professionals they are receiving care from to be more important than the quality of care they receive.40 Providing care closer to people’s home community helps maintain and strengthen trust with the medical system, ultimately leading to better health outcomes.41
Limitations
British Columbia has its own formalized definition of rurality that is not used in other jurisdictions, which limits the generalizability of our findings. However, this could also be a strength, as data that distinguish between varying types of rural sites and provide context to the question of what kind of practice rural general surgeons have are lacking.
Because of the COVID-19 pandemic, there was a provincial decrease in the number of elective surgical cases, which may have influenced the procedures performed in 2020/21.
Finally, the data collected about other specialists working in the RSA-defined rural communities did not consider visiting specialists to RSA communities that provide outreach care, including surgery.
Conclusion
General surgeons who work in rural communities across BC perform a variety of conventional general surgery procedures and unconventional surgery procedures to make surgical care accessible to the communities they serve. Although there is a current trend toward subspecialization, there remains a need for a broad-based rural surgery practice. Our findings highlight the changing landscape of rural general surgery practice, including the decrease in the proportion of unconventional procedures performed over time. This is likely related to changes in postgraduate medical education and resident preferences but also to credentialling policies of regulatory bodies such as the College of Physicians and Surgeons of British Columbia. Further studies may help to elucidate effective strategies for training and succession for surgeons interested in providing rural care as well as to understand the complex policies governing rural surgical care and their implications to those living in these communities.
Acknowledgement
The authors express their sincere thanks to Madeleine Armstrong for her invaluable assistance in organizing data that was integral to this paper’s completion.
Footnotes
Competing interests: Nicole Robbins is chair of a general surgery specialty committee of the Royal College of Physicians and Surgeons of Canada; in this role, she is funded to attend meetings. No other competing interests were declared.
- Accepted November 24, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/