Abstract
Objective: To determine the positive and negative predictive values of visual inspection of peritoneal lavage fluid and the threshold concentration of erythrocytes for diagnosing significant hemoperitoneum by this method.
Design: Nineteen residents in surgery and 21 staff surgeons were asked to inspect mock peritoneal lavage fluid and state whether they would proceed with urgent laparotomy.
Main Results: The overall positive and negative predictive values for visual inspection were 52.0% and 98.9%, respectively. The threshold for diagnosing significant hemoperitoneum by visual inspection was between 10 000 and 20 000 erythrocytes/mL for most subjects. There were no significant differences between residents and staff surgeons.
Conclusions: Visual inspection of peritoneal lavage fluid has good negative but poor positive predictive value, and the threshold for diagnosing significant hemoperitoneum by visual inspection is less than 100 000 erythrocytes/mL. Therefore, patients whose condition is stable and for whom visual inspection of lavage fluid indicates apparently significant hemoperitoneum should not undergo laparotomy without confirmation by laboratory testing.
The diagnosis of significant injury in patients who have sustained abdominal trauma continues to challenge even the most experienced surgeon. In the setting of abdominal trauma, clinical examination alone has an accuracy of 42% to 87%.1,2 Root and colleagues3 introduced diagnostic peritoneal lavage as a rapid and accurate means to determine whether significant intraabdominal injury had occurred, and the criteria indicating significant abdominal injury have evolved since that first study. The initial definition of a positive result, “a faint salmonpink tinge,”3 was ill-defined, and in 1970 Perry, DeMeules and Root4 examined peritoneal fluid microscopically and determined that a concentration of 100 000 erythrocytes/mL was the threshold for predicting significant positive findings at laparotomy. Since then, reviews of quantitative analyses have calculated that the accuracy of diagnostic peritoneal lavage ranges from 93% to 99% with a sensitivity of 85% to 96% and a specificity between 91% and 100%.1,2,5–11
In clinical practice the decision to perform laparotomy is commonly based solely on visual inspection of the peritoneal lavage fluid. In 1972, Olsen, Redman and Hildreth12 attempted to standardize the visual inspection of peritoneal fluid by classifying the fluid from negative to 4+. They also proposed trying to read a newspaper through the tubing as a crude yet convenient method for establishing the result of the lavage. Others, including DuPriest and associates, 7 Parvin and colleagues13 and Bivins and collaborators,14 reported on the gross analysis of the peritoneal fluid as a means to determine positive or negative results. Velanovich11 reviewed articles analysing peritoneal lavage fluid and questioned the use of visual inspection at all. He also stated that quantitative analysis was more reliable than qualitative analysis. Therefore, the true value of visual inspection of peritoneal lavage fluid remains unknown.
Our objectives were to determine the positive and negative predictive values of visual inspection, to determine the visual threshold for diagnosing significant hemoperitoneum and to determine whether experience affects these findings.
Methods
Subjects
The individuals who participated in the study consisted of 19 residents in general surgery and 21 staff general surgeons in the Department of Surgery at the University of British Columbia. Residents from all levels of training from postgraduate years 2 through 6 were represented. The surgeons worked at St. Paul’s Hospital and Vancouver General Hospital and Health Sciences Centre, two university-affiliated teaching hospitals in Vancouver that admit patients with major trauma. The surgeons selected for the study were those who regularly care for trauma patients.
Samples
Whole blood was obtained from healthy volunteers by a syringe and needle technique. The syringe and needle had been coated with Hepalean (1000 U/mL) to prevent coagulation of the blood during processing. The concentration of erythrocytes was determined with a Coulter counter (model STKS; Coulter, Miami Lakes, Fla.). Various volumes of blood were injected into 1-L bags of normal saline kept at room temperature (Abbott Laboratories, Montreal) and mixed to yield six concentrations of erythrocytes. The concentrations desired were 0, 10 000, 20 000, 50 000, 100 000 and 200 000 erythrocytes/ mL. The final concentrations were verified with the same Coulter counter. Intravenous tubing was attached to each saline bag, and the sample was allowed to fill the tubing. A total of 200 mL of fluid was removed from each bag so that the bag contents more adequately represented the amount of fluid obtained from peritoneal lavage, to allow for thorough mixing of the fluid and to obtain fluid for assay to confirm the concentration in each bag. The samples of peritoneal fluid were analysed before and after visual inspection by the subjects and the concentrations compared with Student’s t-test to confirm that significant hemolysis had not occurred over the 4-day period of the study.
Visual inspection
The aims and protocol of the study were explained to the subjects. Adequate lighting, newspaper and a recording sheet were provided. The subjects were instructed to inspect the six prepared saline bags, each bag simulating a diagnostic peritoneal lavage sample obtained from a patient who had sustained blunt abdominal trauma. The subjects were asked to record whether the sample was positive or negative for intra-abdominal injury. A positive result was defined as one that would lead the surgeon to perform urgent laparotomy. Subjects were asked not to compare the bags but to determine a diagnosis for each bag individually.
Analysis of visual inspection results
The results were coded as correct or incorrect relative to the standard criterion for quantitative analysis (i.e., 100 000 erythrocytes/mL). Of the available concentrations, 0, 10 000, 20 000 and 50 000 erythrocytes/mL were negative according to the standard criterion, whereas 100 000 and 200 000 erythrocytes/mL were positive.
We then calculated the number of true positives and negatives and false positives and negatives for the residents, for the staff surgeons and for all subjects combined. Positive and negative predictive values were calculated as follows: positive predictive value = no. of true positives / (no. of true positives + no. of false positives) and negative predictive value = no. of true negatives / (no. of true negatives + no. of false negatives). Accuracy, sensitivity and specificity were calculated as follows: accuracy = (no. of true positives + no. of true negatives) / total no. of cases, sensitivity = no. of true positives / (no. of true positives + no. of false negatives) and specificity = no. of true negatives / (no. of true negatives + no. of false positives). The results for residents and staff surgeons were compared with the Fisher’s exact two-tailed test for proportions.
For each subject, the visual threshold for diagnosing significant hemoperitoneum was determined as the sample with the lowest concentration of erythrocytes that was selected as positive. Again, the results for residents and staff surgeons were compared with Fisher’s exact two-tailed test for proportions.
Results
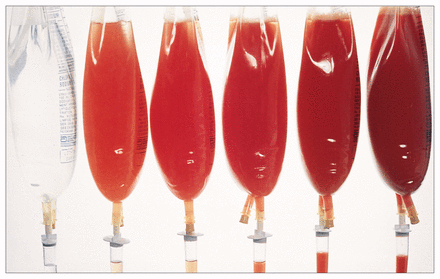
The concentrations of the samples were as follows (mean [and standard deviation]): 12 000 (1000), 22 000 (1000), 50 000 (1500), 100 000 (3500) and 207 000 (3500) erythrocytes/mL. The samples used for visual inspection are shown in Fig. 1. The concentration of erythrocytes in the samples before and after the tests of visual inspection were not significantly different (paired Student’s t-test, p = 0.10). Furthermore, the concentration of erythrocytes in each bag of saline remained stable and did not change on repeat analysis (p = 0.10) over the 4-day period.
Simulated peritoneal lavage samples for visual inspection. From left to right, concentrations are 0, 10 000, 20 000, 50 000, 100 000 and 200 000 erythrocytes/mL.
None of the subjects designated the sample with no erythrocytes as positive, and nearly all of the subjects designated the samples with 100 000 and 200 000 erythrocytes/mL as positive (Table I). In total, 15 (38%) designated 10 000 erythrocytes/mL as positive, 28 (70%) designated 20 000 erythrocytes/mL as positive and 30 (75%) designated 50 000 erythrocytes/ mL as positive.
Number of Residents and Staff Surgeons Who Designated Mock Peritoneal Lavage Samples (at Six Different Concentrations) as Positive for Hemoperitoneum
The calculated positive and negative predictive values are shown in Table II. The overall positive predictive value was 52.0% and the negative predictive value was 98.9%. The values for residents and staff surgeons were not significantly different (p = 0.89 for the positive predictive value and p = 0.50 for the negative predictive value).
Positive (PPV) and Negative (NPV) Predictive Values for Visual Inspection of Mock Peritoneal Lavage Samples Among 19 Residents and 21 Staff Surgeons
Overall accuracy was 69.2%, overall sensitivity 98.9% and overall specificity 54.4%. The values for these calculations did not differ between residents and staff surgeons (p = 0.90 for accuracy, p = 0.20 for sensitivity, and p = 0.90 for specificity).
The most frequent visual thresholds for diagnosing significant hemoperitoneum were 10 000 and 20 000 erythrocytes/mL (Table III). Furthermore, there was no significant difference between residents and staff surgeons for the comparison of subjects with a visual threshold below and above 100 000 erythrocytes/mL (p < 1.0).
Concentration Threshold for Designating a Mock Peritoneal Lavage Sample as Positive for Hemoperitoneum Among 19 Residents and 21 Staff Surgeons
Discussion
Despite new imaging techniques, diagnostic peritoneal lavage remains the key initial diagnostic test for patients who have sustained blunt abdominal trauma. Since its introduction in 1965 peritoneal lavage has maintained its role by being the single test by which the physician can quickly and accurately determine the presence or absence of significant intra-abdominal injury. The diagnostic accuracy of peritoneal lavage has been reported as greater than 95%.1,2,5–11 In clinical practice, visual inspection of peritoneal lavage fluid has been studied as a rapid means of analysis.12–17 There is no doubt that visual inspection is faster.18 However, no study has yet attempted to specify the role of visual inspection. Therefore, we undertook to define the role of visual inspection of peritoneal lavage fluid in the management of abdominal trauma.
We simulated samples of peritoneal lavage fluid to determine the positive and negative predictive values and the visual threshold for diagnosing significant hemoperitoneum. The concentrations chosen were values that have been previously suggested as indicating significant intra-abdominal injury. 1,2,4,19,20 The present standard criteria for blunt abdominal trauma, as accepted by the Advanced Trauma Life Support (ATLS) Program of the American College of Surgeons, is 100 000 erythrocytes/mL.21 This level was originally proposed in 1970 by Perry, DeMeules and Root,4 who found that this was the concentration at which laparotomy findings were almost uniformly positive. Others have suggested alternative values. Hornyak and Shaftan19 in 1979 and McLellan and associates V2 in 1985 suggested 20 000 erythrocytes/mL, as both groups found significant injuries for concentrations between 20 000 and 100 000 erythrocytes/mL. Cox20 in 1984 suggested 50 000 erythrocytes/ mL. In a literature review published in 1987, Gomez and associates1 concluded that 100 000 erythrocytes/mL was still the value with the best accuracy, so we chose that concentration threshold as the one against which to test the value of visual inspection.
We found that visual inspection of peritoneal lavage fluid has a poor positive predictive value (52.0%) but a good negative predictive value (98.9%). In addition, we found that the threshold for diagnosing significant hemoperitoneum among the subjects of the study was far below the standard of 100 000 erythrocytes/mL. The positive and negative predictive values and the visual threshold for diagnosing significant hemoperitoneum did not differ between residents and staff surgeons.
We interpret the positive predictive value of 52.0% to mean that only about half of positive findings by visual inspection will be correct. We interpret the negative predictive value of 98.9% to mean that nearly all negative findings by visual inspection will be correct; thus, visual inspection can serve to rule out significant hemoperitoneum. To our knowledge, no previous study has defined the predictive values of visual inspection of peritoneal lavage fluid.
For most subjects, the threshold for diagnosing significant hemoperitoneum was 10 000 or 20 000 erythrocytes/ mL, far below the present standard criteria of 100 000 erythrocytes/ mL. Similarly, Driscoll, Hodgkinson and Mackway-Jones22 found that some clinicians described suspensions of 10 000 erythrocytes/mL as grossly bloody, and Wyatt, Evans and Cusack23 found that the visual threshold for significant hemoperitoneum was below 100 000 erythrocytes/mL. In the latter study23 the lowest threshold was 2400 erythrocytes/mL. The fact that the visual threshold is far below 100 000 erythrocytes/mL accounts for findings by Drost and collaborators, 16 who described cases in which the visual inspection of fluid so clearly seemed to indicate intraabdominal injury that no laboratory confirmation was sought before laparotomy, the results of which were negative. Therefore, visual inspection without confirmation has led to numerous cases of negative laparotomy.
We also asked whether a learning curve affects the positive and negative predictive values and visual threshold for diagnosing significant hemoperitoneum. We found no differences between residents and staff surgeons with respect to positive and negative predictive values, accuracy, sensitivity and specificity of visual inspection of diagnostic peritoneal lavage. In contrast, Wyatt, Evans and Cusack23 observed a learning curve, senior registrars choosing a higher threshold than registrars. Either the residents in this study had a higher visual threshold or the staff surgeons had a lower visual threshold than their respective counterparts in the study by Wyatt, Evans and Cusack.23
Our study design allowed each subject to use the method that he or she routinely uses for visual inspection of peritoneal lavage fluid. These methods may include inspection of fluid in the tubing or the bag or attempting to read a newspaper through the fluid. The use of different methods of visual inspection may account for the poor positive predictive value. The subjects were allowed to inspect the samples individually; the lack of standards for comparison may also have been a factor. In this regard, Tandberg and colleagues18 have shown that a visual comparison using bedside colorimetry not only allows subjects to correctly determine the presence of significant hemoperitoneum but also allows them to correctly determine the concentration of erythrocytes. It is possible that the positive predictive value for visual inspection could be improved by comparing the fluid with a bedside colour chart for different concentrations of erythrocytes.
We conclude that visual inspection can be used to rule out significant hemoperitoneum. However, we recommend that, provided the patient’s condition is hemodynamically stable, peritoneal lavage fluid that appears positive be sent for quantitative analysis before laparotomy is performed.
Acknowledgments
We thank Ken Cheng for his invaluable assistance in the laboratory.
Footnotes
Presented at the annual meeting of the Trauma Association of Canada, Vancouver, Sept. 9, 1993
Dr. P. Terry Phang holds a scholarship from the St. Paul’s Hospital Foundation.
- Accepted October 11, 1995.