Abstract
A literature review conducted for a 1989 article on assessing the quality of life in surgical studies revealed that quality of life was more often mentioned than measured. Few authors reported the use of known, standardized scales. The objective of this study was to determine if and to what extent this situation has changed. A MEDLINE search of surgical studies published between 1989 and 1995 produced over 277 abstracts of surgical studies containing the words “quality of life.” The abstracts were studied in three time periods: 1989–1990, 1991–1992 and 1993–1995. Findings indicated that the use of the term “quality of life” increased markedly over the study period, and studies using standardized measures escalated from 27.4% in 1989–1990 to 48.3% in 1993–1995. Those abstracts not stating how quality of life was assessed decreased from 48.4% in the early period to 21.7% in the last period. Of the abstracts reporting studies that used quality of life measures, 33% came from cancer studies, 21.7% from cardiovascular or respiratory studies, 14.8% from gastroenterology studies, 13.4% from nephrology studies and 6.1% from orthopedic studies. Surgical investigators selected a variety of global measures of quality of life as well as disease-specific instruments. The abstracts also revealed that surgeons are using quality-of-life assessment to monitor patients over time, to help select patients for surgery, to determine the effects of surgical treatment and for making policy decisions. Notwithstanding the limitations of this project, there is evidence in the literature that surgeons are increasingly willing to assess the impact of the surgical interventions by quality-of-life measures and are becoming more familiar with the diverse measures used to assess quality of life.
From a literature review done in 1989 for a review article1 on assessing quality of life in surgical studies, I and my colleague were left with several impressions. The term quality of life frequently appeared in surgical studies but was more often mentioned than measured. In discussing results, authors noted that quality of life should have been measured or that it should be measured in future studies. Those actually evaluating quality of life tended to use either homemade measures, for which the psychometric properties were unknown, or batteries of scales, each of which assessed a domain thought to contribute to life’s quality. Only a few authors reported the use of known, validated scales that assess quality of life. In particular, few disease-specific measures had been used in surgical investigations.
Recently, when asked to speak about assessing quality of life in surgical practice and research, I began to wonder if, and to what extent, this situation had changed. Information contained in several reviews2–6 suggested that it might have. In an attempt to quantify and describe what had happened, a MEDLINE search of surgical studies containing the term “quality of life” was done. It produced over 300 titles for review. After eliminating editorials, case studies, letters, psychometric studies and review articles, 277 abstracts were available to determine if, and how, quality of life had been assessed.
Method
Each abstract was categorized into one of five groups. To be assigned to the standard group, the abstract had to report that the investigators used a named, reliable, validated measure known to tap the important domains contained in quality-of-life scales. Although no one definition has gained universal acceptance,1,7 quality of life as it relates to health may be thought of as an individual’s subjective perception of his or her physical, psychologic and social well-being after taking into account the impact of disease or treatment.8 It is therefore a multidimensional construct7 incorporating, at least, items assessing personal perceptions of health state and of physical, psychologic, social and role functioning. Some generic measures also include information on spirituality, economic status, expected longevity and opportunity, the advantage or disadvantage experienced by an individual because of health. In addition, disease-specific quality-of-life measures include symptoms and dysfunctions related to the condition under study.
The second category included abstracts in which the authors stated that they had employed a semi-structured or structured interview to gain information about quality of life but failed to name a specific interview schedule. In the third category, the authors reported using a self-administered questionnaire that was sometimes noted as being developed by the investigator for the study. The fourth group of abstracts reported a battery of measures each of which assessed a factor known to be related to quality of life. In these abstracts, scales assessing such outcomes as anxiety, depression, coping ability, exercise tolerance, activities of daily living, pain and nausea were employed. While mood, the presence of symptoms and diminished capabilities to perform activities clearly impact on perceived quality of life, one of these cannot be substituted for its overall measure. Ganz, Schag and Cheng,9 for instance, found that performance status correlated only moderately with quality of life in persons with cancer. The final group of abstracts comprised those in which it was difficult to ascertain if or how quality of life was assessed, but it was mentioned. In an effort to detect trends, the abstracts were also divided into three time periods: 1989–1990, 1991–1992, 1993–1994 plus the first 3 months of 1995.
This methodology has major limitations. First, the denominator of 277 abstracts in no way suggests that only this number of surgical studies during this time span dealt with quality-of-life issues. It simply means that a single database computer search identified the term in the title or abstract in 277 instances. Moreover, the length of abstracts is dictated by editorial policy in each journal. Some were short; others were long. It may be that for space constraints or other reasons, authors omitted names of measures, and as a consequence these abstracts were misclassified. Finally, the time periods were not equal.
Findings
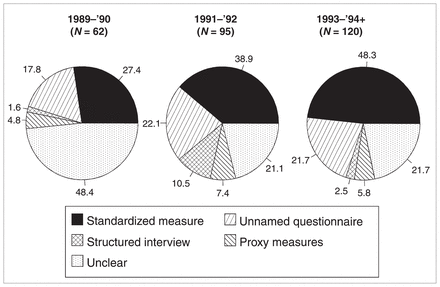
Fig. 1 demonstrates the recent trends in reporting quality of life in surgical studies. First, use of the term appears to be increasing over time, and those studies reporting the use of a known validated measure increased from 27.4% in 1989–1990 to 48.3% in 1993–1995. Those abstracts that were unclear as to if and how quality of life was assessed, decreased from 48.4% in the earliest period to 21.7% recently. The use of a structured interview varied across the time periods. The employment of batteries of measures remained relatively constant (5% to 7%) as did the use of unnamed self-administered questionnaires (19% to 22%).
Trends in reporting quality of life in surgical studies, 1989 to 1995.
Of the 277 abstracts, 33.2% reported studies of patients with cancer, 21.7% involved patients with cardiovascular or respiratory disease, 14.8% came from gastroenterology studies, 13.4% from nephrology studies and 6.1% were studies of patients who underwent orthopedic procedures. The remaining 10.8% came from urology, otolaryngology, plastic surgery and neurosurgery studies.
Surgical investigators selected a variety of standardized generic measures of quality of life. Most frequently chosen were the Nottingham Health Profile,10 the Sickness Impact Profile11 and the Medical Outcomes Study 36-Item Short-Form Health Survey (SF-36).12 These measures were applied to different types of cancer patients and those receiving organ transplants as well as in studies of cardiac and vascular surgery. In addition, researchers selected the McMaster Health Index Questionnaire,13 the Quality of Well-being Scale,14 the Spitzer Quality of Life Index,15 the quality of life index described by Ferrans and Powers,16 The Reintegration to Normal Living Index,17 and the Dartmouth COOP Charts.18 The Performance Status Scale of Karnofsky and Burchenal,19 although acknowledged as not being a comprehensive quality-of-life measure, is still widely employed in cancer and transplantation studies and thus was included. Finally, the use of utility measures20 is on the increase, and they have been selected as outcomes in studies of organ transplantation, joint replacement and abdominal surgery.
Surgeons are also choosing disease-specific quality-of-life measures. Five were used in cancer studies: Functional Living Index-Cancer,21 European Organization for Research and Treatment of Cancer scales,22 Cancer Rehabilitation Evaluation System,23 linear analogue self-assessment scale24 and Quality of Life — Bone Marrow Transplant tool.25 Three others — the Arthritis Impact Measurement Scale,26 WOMAC (Western Ontario and Mc-Master universities) Osteoarthritis Index27 and the Functional Milestone Scale28 were used as outcome measures of orthopedic procedures. The Visick Scale29 and the Gastrointestinal Quality of Life Index30 were applied to patients who underwent abdominal surgery. Urologists assessed outcomes after prostate surgery with use of the quality of life questionnaire for benign prostatic hyperplasia described by Epstein and associates31 and neurosurgeons employed the Epilepsy Surgery Inventory-55.32
Discussion
The situation with respect to assessing quality of life in surgical studies has changed dramatically since the previous review. Moreover, surgeons expressed a variety of reasons to assess quality of life in surgical practice and research. Data from multidimensional quality-of-life assessments provide surgeons with a more comprehensive picture than the often-brief response to the question “How are you feeling?”. This information about an individual patient, especially if gathered serially, may be one of several factors weighed by the surgeon and the patient in deciding when surgery should be performed. Group data about quality-of-life outcomes, assessing specific surgical interventions, should also assist the doctor and patient in selecting which operation to choose,5 since information contained in these outcomes has meaning to patients. It has also been suggested5 that quality-of-life information may reveal important differences between treatment approaches that may be conveyed to patients. One study33 determined that total gastrectomy produced a better quality of life than proximal gastrectomy for gastric cancer. Another randomized trial34 found that amputation for limb sarcoma gave consistently better scores on a battery of outcome measures than limb-sparing surgery with radiotherapy. In other words, when quality of life is the outcome assessed, the results are sometimes not as expected. Discussions about these outcomes may facilitate the decision-making process of patients and their doctors.
Quality-of-life data may also help select patients for surgery in another way. There is mounting evidence that they can predict surgical outcome. Several studies have reported that cancer patients with “high” quality-of-life scores respond more favourably to therapy and seem to have better survival.35–37 Similarly, performance status, as assessed by the Karnofsky Performance Status Scale before transplantation correlated highly with postoperative survival38 and the Nottingham Health Profile was able to discriminate between provisional and definitive candidates wait-listed for heart transplantation.39 Further, patients with “low” mental health scores before minor surgical procedures reported poor outcomes, whereas those with “low” global health scores claimed better success.2 This kind of information can be used in the selection process.
Another reason for assessing quality of life relates to the consensus emerging in the literature that mortality and morbidity, as outcomes of surgery are inadequate in many situations. For minor, day or elective surgery, for comparing minimally invasive and traditional techniques, for palliative procedures, when the procedure is not curative and symptoms or dysfunctions remain, when treatment improves life expectancy but at the expense of greater morbidity and when comparing different treatment approaches especially if survival is similar, quality of life may be the outcome of choice.
In an era of increased accountability, assessing the quality of care provided by an institution or a department is assuming greater importance. Surgeons are being called upon to routinely evaluate their surgical programs, not only in terms of the process of care delivery but also in terms of its outcomes. Clearly of one of the outcomes, important to both patients and those who pay, is an estimate of health-related quality of life.
Finally, quality-of-life assessments are being used to assist in making policy decisions and allocating resources.40 In particular, utility measures such as quality-adjusted life years, which combine measures of quality and quantity of life into a single value, are advocated as a means of analysing the cost-effectiveness and cost-utility of a health care program.20 Although the use of such measures is increasing in surgical studies, more needs to be learned about whether such approaches truly assess the health-related quality of life of patients.
Conclusions
There is evidence in the literature that for many reasons surgeons are increasingly willing to use quality-of-life measures to assess their patients, their practices and the impact of their surgical interventions. Moreover, the surgical community is becoming more familiar with the diverse approaches and measures used to assess quality of life.
Footnotes
Presented at the 3rd World Conference — SEE: Surgical Efficiency and Economy, Kiel, Germany, September 1995
- Accepted March 6, 1996.