Abstract
Gastrointestinal duplication is a rare congenital anomaly. Although it usually presents within the first few years of life, it may appear much later as described in this report of a 19-year-old man who had symptoms of gastric outlet obstruction. He was found to have a noncommunicating antral duplication cyst. The cyst was managed by antrectomy with excision of the cyst and several centimetres of duodenum. Microscopically the duplication cyst contained a mucosa, submucosa and muscularis. There was no evidence of ulceration or malignant cells. His recovery was smooth. The etiology, presentation and management of antral duplication cysts causing gastric outlet obstruction are discusssed.
Gastrointestinal duplication is a rare congenital anomaly that usually presents within the first few years of life. There is a variety of clinical manifestations, depending on the location within the gastrointestinal tract. We describe the case of a 19-year-old man who had no significant medical history but presented with acute symptoms of gastric outlet obstruction. He was discovered to have a large, noncommunicating duplication cyst with gastric mucosa in the antrum of the stomach.
Case report
A 19-year-old man presented with a 7-day history of worsening epigastric pain, nausea and vomiting 1 to 3 hours after eating. He had no history of nausea, vomiting, pain, fever, jaundice, change in bowel habit, abdominal surgery or other significant medical conditions. Physically, he was thin but well developed. He complained of moderate epigastric tenderness. A freely mobile upper abdominal mass was noted. Laboratory evaluation was unremarkable with respect to the blood count, serum amylase level, liver function and urinalysis.
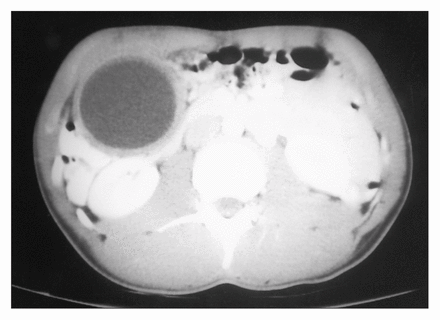
Chest and abdominal plain films were unremarkable. Computed tomography (Fig. 1) with contrast showed a cyst mass measuring 7 × 7 cm. The mass was thought to be located in the duodenum, as demonstrated by contrast surrounding but not within the cystic mass. There was also a central pneumobilia, most likely a result of the mass stretching the ampulla of Vater. The mass was believed to be either a duodenal duplication cyst or a choledochal cyst.
Computed tomography scan showing cystic lesion.
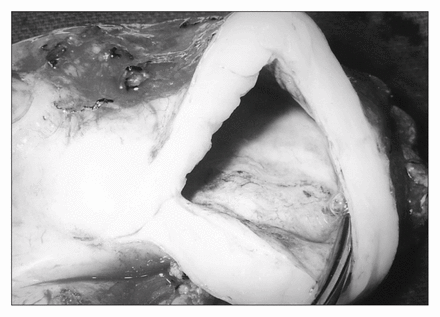
Based on the patient’s symptoms of gastric outlet obstruction and CT findings, we carried out an exploratory laparotomy the next day. A cystic mass measuring 9 cm was noted in the antrum of the stomach along the greater curvature (Fig. 2). Because of the size of the cyst, an antrectomy was performed along with excision of the antral duplication cyst and the first few centimetres of the duodenum. Reconstuction was carried out using the Bilroth I technique. No other cysts or abnormalities were found. Postoperatively, the patient had an uncomplicated recovery.
Gastric duplication.
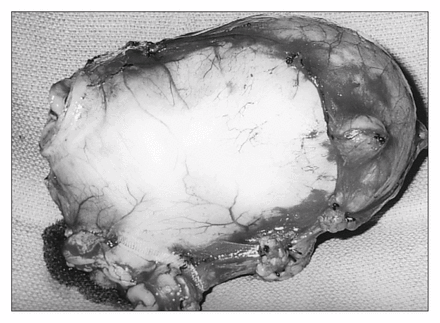
Gross examination of the operative specimen (Fig. 3) showed at 9-cm noncommunicating cystic, distal antral mass along the greater curvature of the stomach. The cyst drained a collection of clear, mucinous fluid. Microscopic study demonstrated a mucosa, submucosa and muscularis. The mucosa was a variant of the gastric type with mucous pyloric-type glands. There were no signs of ulceration or malignancy.
Operative specimen.
Discussion
Enteric duplication is a particularly rare congenital entity in adults; the majority of cases occur in children.1 By definition, a gastrointestinal duplication must have a layer of smooth muscle, be located within or adjacent to part of the gastrointestinal tract and have a mucous membrane lining similar but not adjacent to the segment of the gastrointestinal tract.2 A number of theories have been propounded to explain the embryonic development of gastrointestinal duplications. These include abortive twinning,3 persistent embryologic diverticula that later develop into duplications,4 splitting of the notochord,5 aberrant recanalization of the lumen6 and hypoxic or traumatic events early in fetal developement. 7 No single theory adequately explains all types of duplications.
Duplications can be found anywhere in the alimentary tract from mouth to anus.8 They tend to be more common in females and are sometimes associated with other developmental abnormalities, including a second duplication elsewhere in the gastrointestinal tract. Although the ileum is the most common site,9 involvement of the stomach is the most uncommon, occurring in approximately 4% of all enteric duplications.10 In a composite review of 281 gastrointestinal duplications reported in 4 separate, comprehensive studies, only 21 (7.5%) were located in the stomach. Of those 21, only 1 was reported in the pylorus or distal antrum.11 The majority of stomach duplications are on the greater curvature, 12,13 and are noncommunicating and cystic in nature. Although enteric duplications may contain any type of gastrointestinal mucosa, only gastric mucosa and ectopic pancreatic tissue are clinically significant: they may present with signs of ulceration and pancreatitis. 11 In addition, rare cases of malignant disease within the cyst have been reported.14
According to Hawkins, Lowery and Mullen2 there are 4 common presentations of gastric duplications: pain from distension of the cyst, intestinal obstruction, intestinal necrosis from pressure on mesenteric vessels, and ulceration and hemorrhage.2 The most common physical finding is a palpable mass.15 The diagnosis is suggested by the medical history, a palpable abdominal mass and radiologic detection of an epigastric mass. Although plain films and barium studies may yield the diagnosis, magnetic resonance imaging and CT are needed to assess the nature and size of the mass. The most conclusive evidence, however, is ultrasonographic demonstration of the cyst with a hypoechoic muscle layer and an inner echogenic mucosal layer.11
Therapy for the duplication is surgical. Resection of the entire duplication with a rim of normal stomach is advised. Reconstruction can be performed using Bilroth I and II procedures. This therapy is in contrast to the treatment of duodenal duplication, in which resection can jeopardize the ampulla of Vater, common bile duct or pancreatic duct. Most cystic duplications of the duodenum are treated by surgically creating a window between the duodenal lumen and the duplication cyst.
- Accepted December 4, 1997.