A 76-year-old woman was seen because of increasing pain in and deformity of her right knee. She revealed that when she was 4 years old she had injured her right knee and was hospitalized for some months. After her hospitalization, which did not involve any surgery, she was left with a stiff but painless knee. She stated that her knee was “straight,” by which she meant there was no varus or valgus deformity, but she also stated that her knee was always slightly flexed and could not be further flexed or extended. Despite this she was able to walk unlimited distances and to do hard physical work without any significant knee discomfort.
Approximately 1 year before the current presentation she experienced increasing pain in her right knee. She was seen in consultation by an orthopedic surgeon who had suggested that she would be a candidate for knee replacement surgery and placed her on the waiting list for that operation.
During this waiting period, she suffered increasing discomfort in her knee associated with significant deformity, which she said had progressed rapidly. She was also aware of increased swelling in her knee, but there was no increase in warmth and there was no local tenderness.
On presentation, marked valgus deformity of the knee was noted, with a large knee effusion. There was only a jog of motion in both flexion and extension, but this was extremely painful; the valgus deformity could be corrected to neutral but also was very uncomfortable.
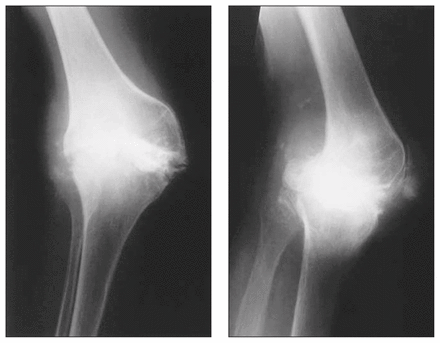
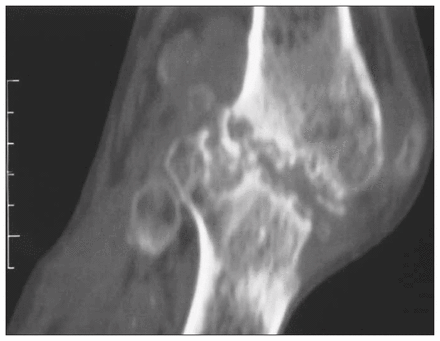
Plain films (Fig. 1) demonstrated a marked valgus deformity with obvious destruction of the lateral compartment of the joint and a relatively well-preserved patellofemoral joint. Computed tomography was carried out to better define the joint surfaces and the degree of bone destruction. The lateral reconstruction view (Fig. 2) showed significant joint and subchondral destruction on both sides of the knee joint as well as adjacent bone erosions.
Anteroposterior (left) and lateral (right) views of the right knee demonstrating extreme valgus deformity and joint destruction.
A lateral computed tomography scan of the right knee, demonstrating bone and joint destruction with erosions on both the femoral and tibial surfaces.
Because of the patient’s history of prolonged hospitalization at an early age and a possible history of pulmonary tuberculosis, a tuberculin skin test was done; the results were positive. A routine culture of aspirated material from the knee yielded no growth, but a culture for Mycobacterium tuberculosis was positive, and this was confirmed by the provincial laboratory.
A knee arthrodesis was carried out combined with triple therapy postoperatively, with a successful outcome.
Bone and joint tuberculosis is relatively rare in Canada today. Although it is occasionally seen in immigrants from areas in which the disease remains endemic and in the Aboriginal people of North America, it should be remembered that reactivation of bone and joint tuberculosis is a possibility at any time. In patients with an unusual clinical presentation of arthritis, especially associated with rapid bone and joint destruction without evidence of purulent infection, granulomatous infection should always be considered.
Footnotes
Submissions to Surgical Images, musculoskeletal section, should be sent to the section editor Dr. Edward J. Harvey, McGill University Health Centre, Montreal General Hospital, 1650 Cedar Ave., Montréal PQ H3G 1A4; edward.harvey{at}muhc.mcgill.ca