What to do when dysplasia is found in patients with ulcerative colitis (UC) has remained one of the most controversial questions in their management. Should one opt for continued colonoscopic surveillance, or proceed to prophylactic colectomy with intent to avoid the development of a colorectal cancer? Despite the experience gained in the management of this disease and reports1 recommending colectomy in patients with high-grade dysplasia (HGD), what ought to be done with patients with low-grade dysplasia (LGD), especially when it is unifocal, remains controversial. As illustrated in this case report, the uncertainty about LGD management is related in part to sampling error, which may underestimate the true extent of LGD in a given case. Management uncertainty is also related to the risk of synchronous or metachronous colorectal carcinoma in the face of unifocal LGD in surveillance biopsies. When a focus of LGD is found, what must be asked is, What is the likelihood that other low-grade foci, high-grade foci or even cancers exist in other areas of the colon not sampled?
Case report
A 44-year-old woman had been followed for a 26-year history of UC. Her disease was documented as a pancolitis. Her symptoms over the last several years were minimal and she had been maintained on a low dose of mesalamine. A recent surveillance colonoscopy identified a focus of LGD and another indefinite for dysplasia; results of the rest of the biopsies taken were negative. She was seen in consultation for proctocolectomy and an ileo-anal pouch procedure (IAPP). The pros and cons of surgery, in the context of the pathologic evidence at hand, were discussed at length.
Three months later, a further surveillance colonoscopy was done with an effort to concentrate biopsies on the left side where her disease was worst, as well as from where the previous biopsies showing dysplasia had been obtained. Despite many biopsies of the entire colon, particularly the left side, no dysplasia was found. Nonetheless, the patient had by then made her decision to undergo IAPP surgery. The colectomy specimen revealed extensive multifocal LGD.
A gastrointestinal pathologist (MG) interpreted both sets of surveillance biopsies and the colectomy specimen.
Discussion
Colectomy versus continued surveillance in patients with longstanding UC is a challenging decision. Several factors must be considered. Often such patients have quiescent disease, making the prospect of major abdominal surgery with a likelihood of poorer function afterward unattractive. On the other hand, the risk of developing colorectal cancer increases with the length of history of UC as well as the amount of colon affected.
A precursor to cancer,2 the finding of dysplasia upon biopsy of the colon in such patients is a significant predictor not only of coexistent cancer but also of their risk of subsequent development of colorectal cancer. With this attendant risk, it is generally accepted that when HGD is found on biopsy, colectomy should be performed.1 What is unclear is what to do if LGD is found, particularly with a single focus only. Practice guidelines put out by the American College of Gastroenterology3 recommend colectomy when LGD is found in a mass lesion or stricture. According to these guidelines, colectomy may also be indicated when LGD is found in flat mucosa. Studies in the USA4 and United Kingdom5 have shown that gastroenterologists usually opt for continued surveillance and not colectomy when LGD in flat mucosa is found.
Recently, however, studies have begun to advocate that patients with LGD proceed to colectomy. Woolrich and colleagues6 showed that LGD, like HGD, is predictive of future carcinoma: of the patients studied, 18% of those with LGD progressed to carcinoma within an average of 6.3 years.6 Bernstein and associates7 found that 16%–29% of patients with untreated LGD progressed to a dysplasia-associated lesion or mass (DALM), HGD or cancer. Of patients with indefinite results on biopsy, 28% progressed to HGD and 9% to cancer.7
When Gorfine8 reviewed the pathology reports of 590 patients who had undergone total or restorative proctocolectomy for UC, 160 had been examined with colonoscopy within 1 year before surgery. Of 11 cases thought preoperatively to have had LGD, 7 were subsequently found to have invasive carcinoma. A solitary dysplastic focus was found in 30 of 77 cases of colectomy where specimens contained dysplasia (40%); 11 cancers were found in association with unifocal dysplasia. Patients with a preoperative diagnosis of LGD were 43 times more likely to have a coexisting carcinoma than those not thought to have dysplasia.
These results suggest that a finding of dysplasia, regardless of whether it is high-or low-grade, should warrant a colectomy. In a study by Ullman and coworkers9 of UC patients with flat LGD who did not undergo immediate colectomy, 50% developed HGD, a raised dysplastic lesion or adenocarcinoma within a median of 32 months. The cumulative risk of neoplastic progression was 33% at 5 years (95% confidence interval 9%–56%). The authors9 thought this rate of progression supported the practice of recommending colectomy for pathologically confirmed flat LGD.
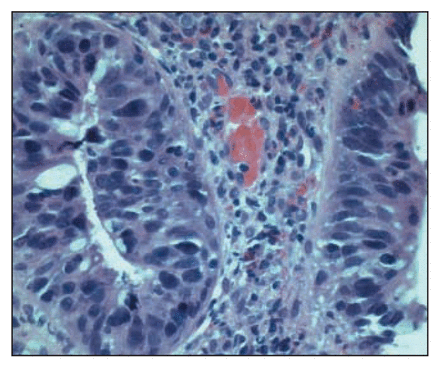
The grading of dysplasia still involves considerable interobserver variability.10 It is therefore important that pathologists interpreting biopsy results be familiar with up-to-date grading schemes, specifically those forming the basis for the latest recommendations. In LGD, nuclei are enlarged, hyperchromatic and limited to the basal half or two-thirds of the cell (Fig. 1). In HGD, nuclear changes are more severe and the nuclei extend into the upper third of the cells (Fig. 2).11 Overall agreement in detecting and grading dysplasia in the setting of UC, even among experienced pathologists, is poor —between 42% and 65%, in one study.12 However, the importance of accurately distinguishing between the various categories in the classification of dysplasia depends on the management algorithm adopted. Distinguishing LGD from HGD is no longer an issue if colectomy is carried out for dysplasia of any grade.
Thin section of large-bowel mucosa showing low-grade dysplasia. Inflammation is present but minimal, and there is enlargement, hyperchromasia and mild stratification of the nuclei of the crypt epithelial cells. Nuclei are seen in the basal one-third of the epithelial cells. Staining is hematoxylin and eosin: left, high-power magnification (× 400); right, low-power (× 200).
High-grade dysplasia in large-bowel mucosa. Inflammation remains minimal, but enlargement, hyperchromasia and stratification of nuclei are more pronounced. There is some loss of nuclear polarity, and some nuclei and mitoses in the epithelial cells are visibly located in the upper one-third (hematoxylin and eosin, × 400).
The distribution of dysplasia is focal in UC. During surveillance colonoscopy, typically less than 1% of the colonic mucosa is sampled.13 To detect any dysplasia present in patients with UC, 33 biopsies have been shown to be required for a 90% sensitivity.14 Given this, it is perhaps not surprising that multifocal LGD was found in the colectomy specimen of the patient reported here, in whom 2 sets of biopsies during dysplasia surveillance identified only 1 focus of LGD and 1 focus indefinite for dysplasia. (In fact, the second surveillance endoscopy failed to reproduce the findings of the first.) It is obviously important to avoid under-representation of the mucosa at dysplasia surveillance. This case is evidence against the practice of continued surveillance of confirmed unifocal LGD. Bernstein15 recommends that endoscopic dysplasia surveillance commence at 8 years of disease. If results indefinite for dysplasia are reported, endoscopy should be repeated within 2 months with an increased number of biopsies. Colectomy is recommended if LGD, HGD or DALM is diagnosed.
Historical recommendations for the management of dysplasia in the patient with UC may reflect the options available at that time. Certainly, current outcomes for the ileoanal pouch procedure are much more acceptable than in the early 1980s.16–18 Now that re-establishment of continuity is the norm for patients who have had a proctocolectomy for UC, we can no longer recommend that such patients risk a possible carcinoma in favour of a few more years of keeping a colon that will eventually almost certainly require removal.
Conclusion
In the last 2 decades, the management of low-grade dysplasia found during follow-up of patients with ulcerative colitis has progressed from continued surveillance to recommendations for colectomy. The increased technical proficiency and reduced morbidity associated with restorative proctocolectomy makes this an acceptable decision for disease management.
Footnotes
Competing interests: None declared.
- Accepted December 22, 2003.