Conventional repair of lesions of the descending thoracic aorta (TA) carries a definite risk of postoperative mortality and serious complications.1 The treatment of a TA aneurysm is more complex when a significant stenosis of the internal carotid artery (ICA) is associated.
Endograft repair is a less invasive treatment method for TA lesions, for which encouraging results have been reported.2–3 It may be assumed that adding simultaneous carotid endarterectomy (CEA) to endograft TA repair will be well tolerated and will not increase the overall risk significantly.
Case report
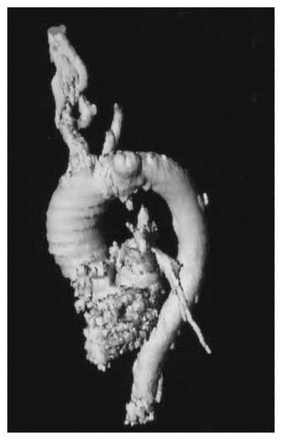
A 76-year-old woman was admitted for an aneurysm of the aortic isthmus 3 cm in diameter. It originated at the edge of the left subclavian artery (SA) ostium and was associated with a left common carotid artery (CCA) arising from the innominate artery as a common trunk (Fig. 1). Duplex ultrasound of the cervical vessels revealed a concomitant 75% stenosis of the left ICA.
Helical computed tomographic (CT) image of the thoracic aorta with 3-dimensional reconstructions. The saccular aneurysm (3 cm in diameter) of the aortic isthmus involves the ostium of the left subclavian artery; the left common carotid artery originates from the innominate artery, as a common trunk.
Her medical history included an accidental fall onto her left flank 3 months earlier.
A conventional angiogram of the aortic arch and supraortic trunks confirmed the left ICA stenosis, and showed the distance between the common trunk and the superior margin of the aneurysm to be adequate for a safe proximal landing of a stent–graft.
The patient was scheduled for left SA to left CCA transposition, left CEA, and stent–graft exclusion of the aneurysm.
At operation, with the patient under general anesthesia, arterial transposition and CEA were performed first. The left SA and proximal CCA were exposed through a supraclavicular incision, and the left carotid bifurcation through a separate, standard presternocleidomastoid incision. The left SA was transposed to the left CCA lateroterminally; the proximal stump of the SA was oversewn, and flow was restored in the distal SA and vertebral artery. An eversion left-CEA was performed, and the 2 wounds were closed.
Subsequently, a 38-mm Talent TPS™ thoracic stent–graft (World Medical Inc., Sunrise, Fla.; Medtronic, Sunnyvale, Calif.) was introduced through the left femoral artery and deployed immediately below the ostium of the innominate artery and just above the ostium of the celiac trunk, while systolic blood pressure was reduced to 70 mm Hg.
The patient’s recovery was uneventful. She was discharged after helical CT imaging showed that the morphology of the arterial reconstructions was correct and free of endoleaks (Fig. 2). At follow-up 6 months later, she was faring well; Doppler ultrasound confirmed that the arterial reconstructions continue to be patent, and repeat helical CT revealed no endoleaks.
Postoperative helical CT image with 3-dimensional reconstructions. Exclusion of the aneurysm is complete; the morphology of the transposition of the left subclavian to common carotid artery and the endarterectomy of the left carotid is correct.
Discussion
The patient presented with an aneurysm of the aortic isthmus of probable posttraumatic etiology. The absence of mural thrombus within the aneurysmal sac and throughout the thoraco-abdominal aorta allowed for the absence of embolization during endovascular manœuvres.
Anatomical variation of her left CCA originating from the innominate artery supported the indication of endovascular repair, as it allowed for a more extensive proximal landing zone of good quality for the stent–graft.
Covering the ostium of a patent left SA with the graft has been reported to be apparently safe.4 Nevertheless, we prefer to initiate a TA endovascular procedure by transposing the left SA and left CCA whenever we anticipate that the ostium of the SA will be covered by the graft. Besides preserving direct vertebral and upper-arm arterial flow, this strategy is used to prevent significant endoleak, which is potentially followed by graft migration, aneurysmal rupture, or both.2
Left SA–CCA transposition carries minimal risk of cerebral ischemia, provided that the contralateral ICA is patent.5 In this setting, the addition of a homolateral CEA was also well tolerated.
Remedy of ICA stenosis concurrent with TA lesions usually requires a staged approach in conventional TA repair. Simultaneous treatment can be considered an additional advantage of stent–grafting of the descending thoracic aorta.
Footnotes
Competing interests: None declared.
- Accepted October 29, 2003.