Traumatic pediatric hip dislocation is such a rare entity that most orthopedic surgeons will see few if any such cases in their careers. Nonoptimal management of such a patient, however, could result in devastating and long-lasting consequences to the child. Timely diagnosis and appropriate use of modern diagnostic imaging technology to assist in decision-making are essential. This is a case of a 24-month-old, otherwise normal baby girl who dislocated her hip while descending an enclosed tubular slide in her father’s lap. The presumed mechanism of injury was similar to a dashboard-type injury for an adult, with direct impact to the knee during the descent with the hip in a flexed and adducted position. Upon exiting the slide, the child was unable to bear her weight.
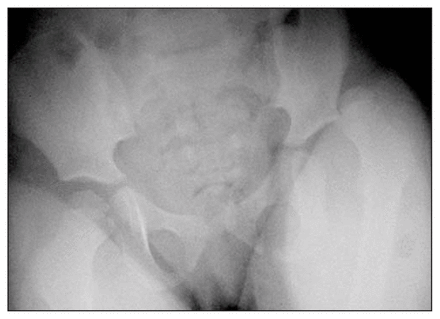
In the emergency department, the child was holding her leg in the classic flexed, adducted and internally rotated position. The femoral head was palpable posterolaterally. Neurovascular examination of the leg was normal. Radiographs were taken immediately (Fig. 1). Reduction was made in a closed manner under general anesthesia within 90 minutes of the injury.
Radiographs taken immediately after the injury reveal a posterolateral dislocation of the hip in this pediatric patient. This injury is very rare in children.
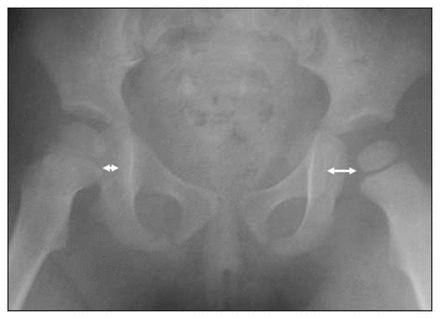
Intraoperative radiographs confirmed reduction, but a fairly concentric 2–3 mm of lateral subluxation was noted (Fig. 2). The joint was taken through a full range of motion (ROM) and found to be stable. Postreduction radiographs, however, revealed 5 mm of lateral subluxation. An unsuccessful arthrogram was attempted through a medial approach at that time, although aspiration of 2 mL of blood was accomplished. A CT scan the following day confirmed lateral subluxation, but no associated fracture or interposed bony fragment was visible.
Postreduction radiographs reveal concentric reduction, with a persistent lateral subluxation of the hip nonetheless. White markers indicate the increased joint space within the reduced hip.
Concern over the possibility of interposed soft tissue prompted gadolinium-enhanced magnetic resonance imaging (MRI) at 48 hours after the injury (Fig. 3). This revealed edema in the surrounding posterior tissues, but an otherwise normal hip joint with no evidence of interposed tissue. A plain radiograph done the same day now showed complete concentric reduction (Fig. 4).
Coronal magnetic resonance image 2 days after reduction. The previous lateral subluxation has resolved and the joint is congruous and located. No soft-tissue interposition is present.
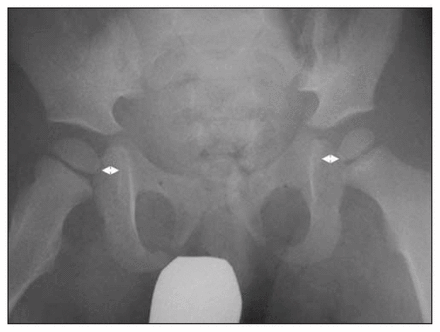
Radiographs 2 days after reduction show improvement in the preceding subluxation; the hip joint is congruous and located. White markers measure equal medial joint spaces.
The patient was discharged home the next day with a modified abduction splint and instructions not to weight-bear. Follow-up radiographs at 1 week confirmed concentric reduction, and her hip ROM was virtually pain-free. One year after the injury, her clinical exam and radiographs were normal, with no evidence of avascular necrosis.
The change from the CT image at 12 hours after injury to the MRI at 48 hours was thought to be secondary to resorption of hemarthrosis. In adults, some form of associated fracture usually occurs with a hip dislocation. A CT image is helpful for determining the interposition of bony fragments. In pediatric hip trauma, however, lax ligaments and predominance of cartilage often lead to isolated hip dislocation.
It is well recognized that soft-tissue interposition in the form of torn or redundant capsule and inverted labrum can be important problems, leading to open exploration. Posttraumatic hemarthrosis mimicking soft-tissue interposition is not well documented in the literature. Based on the CT image, open exploration for soft-tissue interposition could have been entertained in this patient. MRI is best suited for investigation of this problem, and perhaps should be the primary imaging modality for nonconcentric posttraumatic hip reductions. In adult hip dislocations, CT imaging is considered, after radiographs, the immediate diagnostic tool of choice; in traumatic pediatric hip dislocations, MRI may fill this role more effectively.
Footnotes
Submissions to Surgical Images, musculoskeletal section, should be sent to the section editor: Dr. Edward J. Harvey, McGill University Health Centre, Montreal General Hospital, 1650 Cedar Ave., Montréal QC H3G 1A4; edward.harvey{at}muhc.mcgill.ca
Competing interests: None declared.