Spontaneous peripheral and visceral embolization from diffuse, aortic atherosclerotic disease is unusual. It is due to multiple, ulcerated, atherosclerotic plaques, which are lined with thrombus of the thoracoabdominal aorta, and is associated with an irregularly spiculated shape of the aortic wall at angiography and CT, known as the “shaggy aorta” syndrome.1,2
Case report
A 65-year-old man was referred for bilateral, painful cyanosis of the toes, of sudden onset. He was taking warfarin for a previous aortic and mitral valve replacement and aortocoronary bypass grafting 2 years earlier. On physical examination, “blue toe” syndrome, with normal pedal pulses, was evident bilaterally.
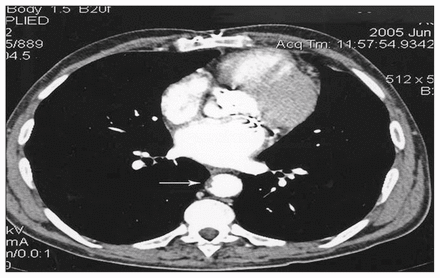
A transesophageal echocardiogram excluded the presence of valvular or intracavitary embolism. Multislice CT showed irregular atherosclerotic plaques, lined with thrombus in the descending thoracic and infrarenal aorta as well as in the iliac arteries, without significant stenoses (Fig. 1). Because the visceral aorta, from the celiac trunk to 2 cm below the renal arteries, was free of disease, we decided to exclude the thrombus in the descending thoracic aorta with a stent graft and to perform a standard, excluding aortobifemoral bypass. The stent graft (Zenith Endovascular Graft; Cook Group Inc., Bloomington, Ind.) was first inserted through the left common femoral artery and deployed from below the left subclavian artery to the diaphragm. Then a standard, Dacron, aortobifemoral bypass graft, originating 1 cm below the renal arteries was inserted. The common femoral arteries were both ligated immediately above the distal anastomoses of the graft. A postoperative CT scan showed satisfactory exclusion of the diseased aorta (Fig. 2).
Multislice CT scan of the thoracoabdominal aorta. The descending thoracic aorta ulcers of the intimal surface are lined with irregular and unstable thrombus.
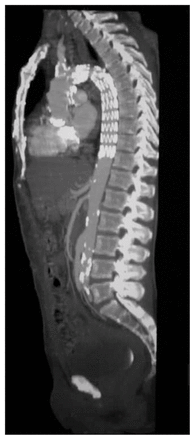
Control, multislice CT scan of the thoracoabdominal aorta, showing the correct morphology of the thoracic aorta stent graft and patency of the aortobifemoral bypass graft.
The patient’s pain resolved and the pedal lesions healed. He was discharged home with a prescription for oral warfarin. At 26-month follow-up, he was well and had had no further embolic episodes.
Discussion
Diffuse atheromatous embolization from aortic atherosclerotic disease is a poorly understood disorder. Many patients showing diffuse multiple thrombus lining along the aortic wall on CT and angiography never experience embolic episodes. “Shaggy aorta” syndrome is associated with both ulcerated, thrombus-lined lesions and clinically evident, repeated embolic episodes. It represents a more aggressive clinical entity than simple aortic atheromatous degeneration or thrombuslined aneurysmal disease.1,2 Diffuse embolization can cause progressive renal failure, pancreatitis, bowel infarction and lower extremity ischemia. Antiplatelet therapy is of unproven efficacy, and anticoagulation is contraindicated, as it probably hinders healing of ulcers thus enhancing instability of aortic plaques and promoting distal embolization.3 Arteriography is also contraindicated as a catheter passed within the aorta can easily “rake off” atheromatous debris, precipitating embolization.1 In our case, distal embolization was likely favoured by prolonged warfarin treatment, which may have led to progressive instability of atheromatous aortic disease.
There is no really effective medical treatment for the “shaggy aorta” syndrome. Prosthetic replacement of the whole diseased aorta provides effective treatment against recurrent embolization. However, given the frequent involvement of the thoracoabdominal or suprarenal aorta, its substitution with prosthetic grafts is associated with high morbidity and mortality.1 Axillofemoral bypass with ligation of external iliac arteries above the distal anastomoses has been proposed as an alternative to aortobifemoral grafting, whenever thoracoabdominal prosthetic substitution is not feasible.1
In our case, the disease involved the descending thoracic and infrarenal aorta, but spared the visceral aorta. Therefore the simultaneous stent grafting of the descending thoracic aorta and standard aortobifemoral bypass allowed complete exclusion of all embolic sources and safe resumption of oral anticoagulation, which was required because of the heart valve replacement.
Footnotes
Competing interests: None declared.
- Accepted February 3, 2006.