Hydatid disease is most commonly caused by Echinococcus granulosus, in which humans are an intermediate host,1 and is endemic in the Mediterranean region, including Turkey, the Middle East and the Far East.2 The disease occurs in the liver in 70% of cases, the lungs in 25% of cases, and at other sites such as the spleen, kidney, pancreas, brain, ovary, mesentery, pancreas, vertebra and soft tissue of the neck.3 Anaphylactic shock, cyst infection of the biliary tree and rupture into the peritoneum are the most severe complications. We report an unusual case of primary mesenteric hydatid cyst perforating the small intestine and presenting as acute abdomen.
Case report
A 19-year-old man presented after 3 hours of abdominal pain, nausea, vomiting and fever. The pain was diffuse but was most severe in the lower quadrant. There was no history of trauma. He had a temperature of 38.5°C, his pulse rate was 110 beats/min and his blood pressure was 100/70 mm Hg. On examination his abdomen was diffusely tender, particularly in the lower quadrant, with guarding and rebound tenderness. Laboratory investigations revealed a leukocyte count of 16.0 × 109/L, with normal hemoglobin level and platelet count. Other electrolyte levels (urea nitrogen, creatinine, transaminases, alkaline phosphatase) were all in the normal range. There were no abnormalities on abdominal radiography. Abdominal sonography showed a moderate amount of fluid in the abdominal cavity and an 8 × 10-cm cystic mass in the lower quadrant.
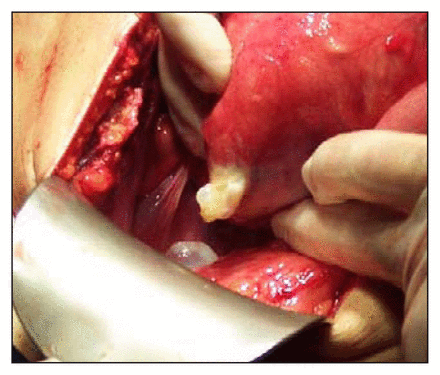
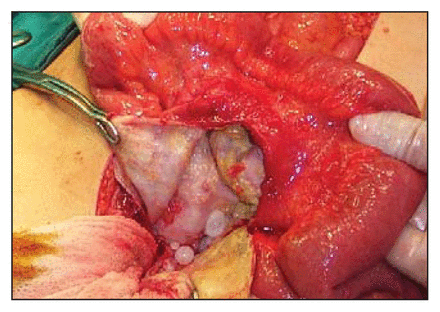
Exploratory laparotomy revealed a cystic mass of the ileal mesentery that measured 8 × 8 × 10 cm. The mass had perforated the mesentery (Fig. 1), and there was fluid in the abdominal cavity. Partial cystectomy was performed and daughter cysts were removed from the abdomen (Fig. 2). The abdominal cavity was washed with 10% povidine-iodine. After a thorough peritoneal lavage, the abdomen was closed with a drain in situ. The patient’s recovery was satisfactory and he was treated with albendazole for 6 months.
Hydatid cyst perforating the mesentery.
Daughter cysts.
Discussion
Hydatid disease is caused by E. granulosus, Echinococcus oligarthrus and Echinococcus multilocularis, but most commonly E. granulosus.4 The disease usually involves the liver and lungs. Uncomplicated cysts are usually asymptomatic. The symptoms are commonly related to complications and vary with regard to the location of the hydatid cysts. In our case, in keeping with the location of the cyst, the abdomen was tense and tender, especially in the lower quadrant with guarding and rebound tenderness. Sometimes, clinical findings can mimic other abdominal disorders. Turdibaev and colleagues5 reported a case of rupture of an echinococcal cyst of the small intestinal mesentery simulating acute appendicitis. Anaphylactic shock due to spontaneous or traumatic cyst rupture or during surgery is a rare and severe complication. We did not encounter anaphylactic reactions in our nontraumatic patient.
Hypertonic saline, 10% povidineiodine, alcohol silver nitrate or cetrimide can be used to irrigate the cyst cavity and the operation area. We used 10% povidine-iodine for our case. Albendazole therapy is the mainstay of treatment in the majority of patients with hydatid disease.1 Our patient was prescribed albendazole (10 mg/kg daily) for 6 months.
Morbidity and mortality in patients with perforated hydatid cyst are higher in those with nonperforated cysts.2 So, especially in endemic areas, hydatid perforation should be considered in trauma patients and patients presenting with acute abdomen.
Footnotes
Competing interests: None declared.
- Accepted September 25, 2006.