We report a rare case of esophageal perforation resulting from a closed traumatic injury that caused hyperextension–flexion of the cervical spine.
Case report
A healthy 76-year-old man sustained closed head and neck trauma after falling down 8 stairs. Over the following days he became febrile, his voice changed and he had difficulty swallowing. Thoracic CT in a local hospital revealed pneumomediastinum. On transfer to our medical centre, he was in stable condition, afebrile, had no subcutaneous emphysema and had a normal leukocyte count. Findings on barium swallow were in the normal range. A broad-spectrum antibiotic was prescribed. Shortly thereafter the patient became septic and was taken to the operating room. A right thoracotomy was performed. Pus was found under pressure in the posterior mediastinum around the entire esophagus, contained by the mediastinal pleura. The mediastinal collection was drained. The thoracic esophagus appeared congested, but no perforation was found.
Because of the mechanism of injury, we decided to explore the cervical esophagus. No injury was found, but a prominent cervical spine osteophyte was identified, which we believe was responsible for the microperforation of the esophagus that resulted in mediastinitis. Neck hyperextension was the most likely mechanism of esophageal injury.
An orthopedic surgeon was consulted with a view to removing the osteophyte, but it was decided that such an action might result in osteomyelitis. We noticed the absence of the intervertebral C6–7 disc as a result of osteophyte involvement and spinal necrosis associated with mediastinal infection. The posterior mediastinum and the cervical area were irrigated with saline and widely drained.
On follow-up 1 and 6 months after surgery, the patient was asymptomatic.
Discussion
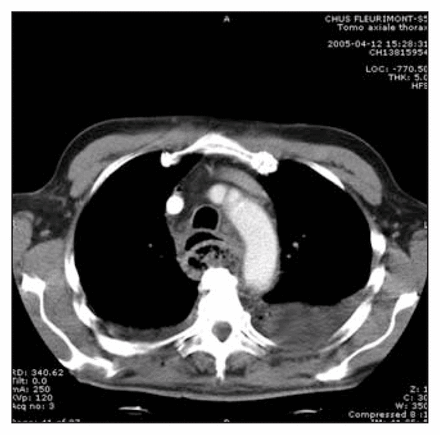
Delay in the time from trauma to definitive management has a significant influence on the development of complications related to esophageal injury; Asensio and associates1 reported that a 12-hour delay led to more such complications and a longer mean stay in the intensive care unit and hospital. In our case there was a 7-day delay between injury and definitive surgical treatment. The initial symptoms were not clear; probably the fever and the infection were related to the patient’s age and immune status. The CT findings of esophageal rupture and mediastinitis included air in the soft tissues of the mediastinum, abscess formation and pleural effusions (Fig. 1). Esophageal perforation has traditionally been considered a life-threatening event with death rates of 10%–40%.2 Most surgeons and recent reviews have favoured an aggressive surgical approach to this condition, including primary surgical repair and esophageal exclusion, drainage, primary esophageal resection and cervical esophagostomy.3 Conservative treatment is controversial, and in most cases the management is surgical. In our case and in the report of Stringer and colleagues, 4 hyperextension–flexion injuries of the cervical spine proved to be a rare cause of esophageal perforation. In our patient the mechanism may have been impingement of the esophagus against an exostosis at the edge of the C6–7 vertebral body. In other cases, entrapment of the esophageal wall between the vertebral bodies occurs as hyperextension changes to flexion. The prevalence of cervical spine injuries remains high in elderly patients, with odontoid fractures being common. A Canadian study found an odds ratio of 3.7 for the clinical variable of age greater than 65 years, and proposed cervical radiography and CT in alert, stable trauma patients.5 The mechanism is illustrated in Figure 2. If not detected and treated early, the perforation may cause mediastinitis, retropharyngeal abscess, sepsis and death.
CT scan shows air in the mediastinal soft tissues, abscess formation and pleural effusions.
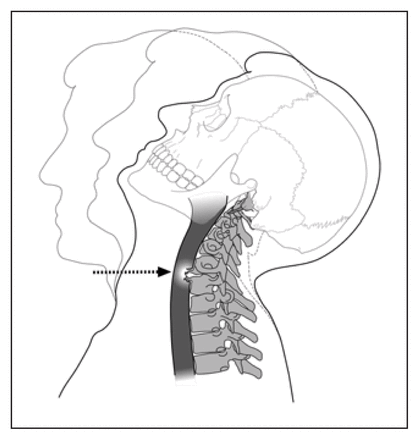
Perforation of the esophagus resulting from flexion–hyperextension in closed traumatic injury.
Early recognition of this complication, with attention to abnormal regional and general clinical signs, is helped by a thorough CT. Early diagnosis is essential in order to prevent a devastating outcome.
Footnotes
Competing interests: None declared.
- Accepted May 17, 2006.