Abstract
Background: Patient esthetic satisfaction related to scarring after orthopedic surgery was rarely assessed before the development of the Patient Scar Assessment Scale (PSAS). The purpose of our study was to translate and validate the PSAS and assess the psychometric properties of the French version.
Methods: We conducted a staged validation with forward and backward translation and concurrent validation. The validation committee comrpised bilingual experts. The patient validation sample comprised 53 orthopedic surgery patients who were assessed at a minimum of 1 year postoperatively. We followed a standardized process for cross-cultural adaptation to develop and assess the French version. First, 2 independent translators completed the forward translation of the PSAS and then met to achieve a consensus version. This consolidated version was then backward translated into English and cross-verified with the original version. A group of orthopedic and plastic surgeons assessed this version for content validity. We assessed the test–retest reliability of the new French scale, which was filled out twice by a cohort of 53 patients, using scale distribution analysis, internal consistency (Chronbach α) and absolute agreement (intraclass correlation coefficients [ICC (2,1)]).
Results: The level of agreement on the translation process between the translators initially and then later among the expert panel was high. The reliability of the translated version (PSAS-Fr) and its internal consistency was high (Chronback α 0.87–0.98 for each of the 6 questions), and the test–retest reliability was excellent (ICC 0.96). On the other hand, there was no bias between occasions (retests difference −0.24) and the scores fell within 2 standard deviations of 5. Older patients had higher satisfaction about scar appearance.
Conclusion: The PSAS-Fr was successfully translated from the original English version and demonstrated strong cross-sectional psychometric properties. Further assessment in longitudinal studies is warranted.
The appearance of the upper extremity and in particular surgical scars is more important to patients than the medical community often appreciates. Studies in patients with rheumatoid arthritis indicated that both men and women were equally concerned about the appearance of their hands, although physicians assumed that it mattered most to women.1 This discrepancy suggests that surgeons and patients have different perceptions of physical appearance. Also, it has been suggested that a surgeon failing to appreciate a patient’s perception of a scar could contribute to legal action.2 The importance of taking into account patients’ opinions of their scars has been recognized,3 and the same study confirmed that patients and health care providers do not agree on the appearance of scars. Paradoxically, most of the studies that compare different types of incisions predominantly take into consideration the treating team’s opinion4–6 instead of the patient’s opinion.
Studies that have compared minimally invasive surgery and standard surgery have rarely evaluated patients’ satisfaction with cosmetic appearance. Satisfaction was most often evaluated when the scar was on the breast or on a more visible portion of the body such as the neck following a thyroid lobectomy.7–10 Some of these authors used a 10-point numeric rating scale ranging from barely satisfied to excellent.8,9 In comparison, relatively little attention has been directed toward studying patient aesthetic satisfaction after orthopedic surgery.11,12 To address this problem, the Patient Scar Assessment Scale (PSAS) was published by Draaijers and colleagues;13 it is a validated 6-item questionnaire designed to measure patients’ satisfaction about their scars.
The purpose of our study was to translate the English version of the PSAS to make it appropriate for a French Canadian audience and assess the psychometric properties of the French version.
Methods
The PSAS
The Patient Scar Assessment Scale is a validated questionnaire published in 2003 by Draaijers and colleagues13 (Appendix 1). It is a simple 6-item self-report scale in which items are scored on a numeric rating of 0–10. The authors used the PSAS to assess 49 scar areas measuring 3 × 3 inches that were caused by a burn injury. The study involved 20 patients aged 15–73 years whose injuries were evaluated an average of 43.7 months after a burn accident. They reported an internal consistency of 0.76.
Patient demographic information
Correlation table for each specific question
Questionnaire: patient scar satisfaction*
Translation process
In the present study, we followed the essential methodological steps recommended by internationally recognized publications involved in scale translation and cultural validation14,15 (Box 1). The first stage consisted of a forward translation completed by 2 independent professional translators, yielding 2 initial French versions (named T1 and T2). The translators then synthesized the 2 versions to create a consensus version (named T1+2Fr). Next, 2 different independent translators completed a backward translation of T1+2Fr. Finally, an expert committee composed of 5 bilingual professionals (2 orthopedic surgeons, 1 chief resident in plastic surgery, 1 research nurse and 1 medical student) reviewed and compared the final French translation and the back translations to obtain a final version.
Guideline for the process of cross-cultural adaptation of self-report measures*
Stage 1: Translation
2 translations (T1 & T2)
into target language (French)
informed + uninformed translator
Stage 2: Synthesis
synthesize T1 & T2 → T1+2Fr
resolve any discrepancies with translators’ reports
Stage 3: Back translation
2 English-language translators
naive to outcome measurement
work from T1 + 2Fr version
create 2 back translations, BT1 & BT2
Stage 4: Expert committee review
review all reports
methodologist, developer, language professional, translators
reach consensus on discrepancies
produce prefinal version
Stage 5: Validation
n = 30–40 (recommendation)
complete questionnaire
probe to get an understanding of item
↵* Adapted with permission from Beaton DE, Bombardier C, Guillemin F, et al. Guidelines for the process of cross-cultural adaptation of self-report measures. Spine 2000;25:3186-91.
The number of patients needed to validate a scale is usually 30–40. Recommendations have also been made to use 5–10 patients per item. As the PSAS comprises 6 straightforward items, 30 patients would be sufficient for validation.14 Accurate estimation or reliability assuming underlying high reliability might require 35–45 patients.16
Participants and setting
We recruited volunteers from an orthopedic clinic who had undergone an orthopedic procedure more than 1 year before we began our study. The clinic was located within a university-based hospital with a level-1 trauma centre. Initially, we sent out 119 questionnaires. We selected patients in a random fashion from the hip and knee, trauma, spine and upper limb clinics. We asked all patients to fill out the questionnaire twice: once on the visit day and once 1 week later at home; the second questionnaire was returned by mail. We excluded from our analysis those patients who completed only 1 questionnaire and those whose demographic information was not concordant from the first to the second questionnaire. To ensure the process was anonymous, we did not use names as identifiers, only demographic characteristics; thus, it was impossible to match responses where this information was discordant. We collected minimal information on the date of surgery and location of their scars as well as age and sex. The ethics committee at our institution approved our study, and each patient provided informed consent.
Statistical analysis
We calculated descriptive and analytical statistics using SPSS 16.0 (SPSS, Inc.), and we analyzed the distribution of scores graphically. We computed correlations between age and time since surgery with PSS scores using a Pearson r, and we performed an analysis of variance (ANOVA) to analyze differences between male and female responders. We evaluated internal consistency using a Cronbach α, and we considered a value greater than 0.70 to be satisfactory.17,18 We evaluated each question in relation to the instrument as a whole. We estimated the test–retest reliability using the intraclass correlation coefficient (ICC) and confirmed internal consistency by Cronbach α. We computed the absolute error (and 2 units of standard deviation [SD]) across the range of scores according to the method described by Altman and Bland.18
Results
Participants
Of the 119 patients who received questionnaires, 29 chose not to complete any questionnaires and were excluded; they provided no reason for nonresponse. We excluded 19 patients because they completed only 1 questionnaire and another 18 patients whose demographic information was not concordant from the first questionnaire to the second. The final sample for psychometric analysis comprised 53 patients who successfully filled out both questionnaires.
Cross-cultural adaptation
There was good agreement on the forward English-to-French translation, and the backward translation to English that was compared with the original version and reviewed by the expert committee of bilingual professionals required only minimal changes. We pretested the resulting version with a small group of 5 patients to ensure that the questionnaire format was comprehensive, and only 1 question was adapted. The final version of questionnaire can be found in Appendix 2.
Échelle de satisfaction du patient : cicatrice chirurgicale*
Validation study
The sociodemographic characteristics of patients are described in Table 1. Participants’ PSAS scores crossed the spectrum of the scale with a tendency toward low scores, consistent with the long follow-up interval (mean score 12.0, SD 9.0). Correlation between age and score was significant. Younger patients reported lesser satisfaction (higher score) than older people (Pearson correlation coefficient −0.47, p = 0.001) There was no significant difference in PSAS scores between male and female patients (11.5 v. 12.2).
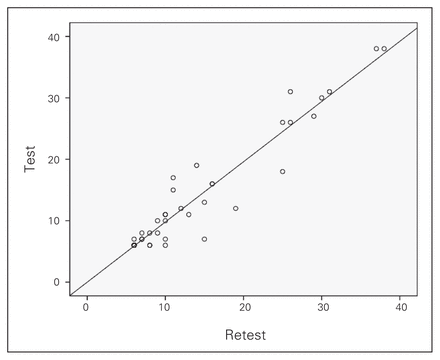
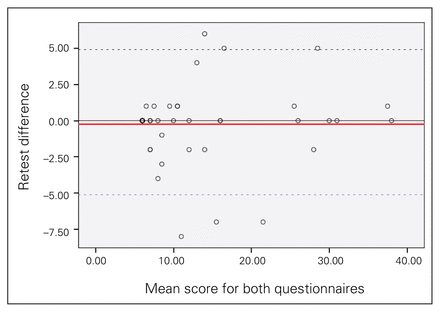
The internal consistency as indicated by Cronbach α was high at 0.98 (95% confidence interval 0.97–0.99) (Fig. 1). We also calculated correlation for each question (Table 2). Test–retest reliability was excellent (ICC 0.96). The mean error across test intervals was negligible at −0.28, and the 2-SD range was −5.21 to 4.67 (Fig. 2).
Correlation of the global score on the Patient Scar Assessment Scale, French Canadian version (PSAS-Fr), initially (test) and 1 week later (retest). The slope corresponds with the correlation coefficient (0.980).
Score distribution using Altman and Bland’s technique.18
Discussion
Our study established a successful translation of the PSAS for a French Canadian audience. An expert panel verified the content validity of the PSAS-Fr, and it was shown to have high retest reliability and low absolute margins of error. The reliability coefficients compare favourably to the original English scale or to other self-report scales translated into French.19–22 We attribute the high reliability obtained by the test–retest method to the simplicity of the original questionnaire and the stability of scar appearance in the same patient at a 1-week interval more than a year after surgery. The data on individual items did not indicate any question to be problematic: all of them showed a correlation coefficient greater than 0.7. An interesting finding is the correlation between age and higher satisfaction related to surgical scars. An explanation could be that older patients had fewer hypertrophic scars.23 Studies on other potential confounders (e.g., scar location, time interval since surgery, type of closure used, presence of traumatic wound) must be completed before we can conclude with certainty that age is related to scar satisfaction.
The limitations of our study include the fact that not all questionnaires were returned owing to our process of not collecting patient identifiers. This anonymous process protected confidentiality but meant that we were unable to resolve returned questionnaires with discordant demographics or area of scar information. We chose to eliminate these conflicting responses from our analysis to be confident of our data integrity. We are unable to determine the effects of these nonresponses on our estimates of reliability. Owing to the anonymous process, it was impossible for us to verify the reason for these reporting discrepancies. A further limitation of our study was that it was cross-sectional and did not evaluate the responsiveness of the scale to detect differences over time.
Despite these limitations, our study supports the use of this tool for surgical research in a French Canadian population. We recommend that future surgical studies where scars are an issue should incorporate this new PSAS translation. Patient satisfaction with surgical scars could be influenced by length, localization, width or texture. This information could be useful when choosing the surgical approach. For example, the assumption of higher satisfaction for mini-incision surgery could be verified by using this scale in English and French Canadian studies. Also, additional studies addressing the psychometric properties in acute populations and in longitudinal cohorts should be conducted to assess responsiveness.
Acknowledgements
J.C. MacDermid’s work is supported by a New Investigator Award from the Canadian Institutes of Health Research. The authors thank Amélie Bourget (plastic surgeon), Pierre Beaumont (orthopedic surgeon), Kathleen Beaumont (translator) and Marie-France Poirier (research coordinator).
Footnotes
Competing interests: None declared.
Contributors: All authors designed the study, wrote and reviewed the manuscript and approved the final version for publication. Ms. Deslauriers and Dr. Rouleau acquired the data, which Drs. Rouleau, Alami and MacDermid analyzed.
- Accepted February 2, 2009.