Abstract
After surgical resection for rectosigmoid carcinoma a 63-year-old man had secretory diarrhea causing severe metabolic acidosis, hypokalemia, hypercalcemia and dehydration. Subsequent investigations revealed a mass measuring 4 × 5 cm in the uncinate process of the pancreas and an elevated vasoactive intestinal polypeptide concentration. The diarrhea responded to treatment with the somatostatin analogue, Sandostatin, and remained under control during a prolonged preoperative period. The patient underwent a Whipple procedure with immediate lessening of his diarrhea. This report illustrates a classic case of vipoma and demonstrates the need to consider this condition in the differential diagnosis of secretory diarrhea, even in the presence of other gastrointestinal lesions. The effectiveness of somatostatin analogues in stabilizing the diarrhea preoperatively is also well illustrated.
Profuse watery diarrhea capable of causing circulatory instability is a known hormonally mediated effect of pancreatic neuroendocrine tumours that secrete vasoactive intestinal polypeptide. Surgical resection provides the only possibility of cure, and recent developments in somatostatin analogues have helped to stabilize these patients preoperatively.
Case report
A 63-year-old man was first seen in Sault Ste. Marie in December 1992, complaining of a change in bowel habit. Stools had become more frequent and looser but with no observable blood or mucus. Colonoscopy revealed a polypoid carcinoma in the sigmoid colon, 20 cm from the anal verge. Uncomplicated anterior resection of a Dukes’ stage A rectosigmoid carcinoma was performed.
Postoperatively the patient continued to have voluminous (up to 8 L/d), painless, non-bloody diarrhea. No organisms were grown on stool culture and no Clostridium difficile toxin was detected. The diarrhea did not respond to treatment with loperamide or cholestyramine resin. Colonoscopy revealed only a sessile villous adenoma 1.5 cm in dimension in the ascending colon. The patient had upper gastrointestinal bleeding, found by endoscopy to be due to peptic esophagitis, and was treated with histamine blocking agents.
The patient was readmitted to hospital on several occasions with severe dehydration and metabolic abnormalities: hypokalemic, hyperchloremic, metabolic acidosis. The blood pH was 6.9 and the bicarbonate level was less than 10.0 mmol/L, with a normal anion gap. He was also hypercalcemic (serum calcium greater than 3.0 mmol/L) and was treated with biphosphonates.
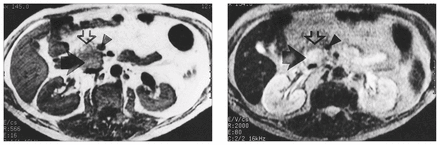
Subsequent investigations, including computed tomography (CT), revealed a mass in the uncinate process of the pancreas. Magnetic resonance imaging (MRI) confirmed the presence of an enhancing mass in the inferior aspect of the uncinate process, which was isointense with T1 weighting and hyperintense with T2 weighting (Fig. 1).
(Left) Magnetic resonance image shows 3.5-cm mass lesion situated within uncinate process of pancreas (black arrow). Mass was isointense with T1 weighting. Open arrow shows normal pancreatic tissue. Superior mesenteric vein (arrowhead) is well visualized. (Right) T2-weighted spin-echo sequence at same level as in Fig. 1 gave hyperintense signal, in keeping with underlying diagnosis of islet cell tumour.
On the basis of the patient’s clinical course and the presence of a pancreatic mass, a clinical diagnosis of pancreatic cholera was made and Sandostatin (Sandoz Canada Inc., Whitby, Ont.) (100 μg subcutaneously) was given three times daily. There was immediate improvement in the diarrhea. The serum VIP level was markedly elevated (228 pg/mL, normal less than 75 pg/mL), confirming the diagnosis of a vipoma. Because he was markedly malnourished, total parenteral nutrition was begun and he was transferred to the Sunnybrook Health Science Centre.
After transfer he was found to have a right lower lobe pneumonia, secondary to aspiration, that developed during transport. His pneumonia progressed to an empyema requiring thoracostomy drainage. Because of this, the preoperative period was prolonged, with episodes of systemic sepsis requiring treatment in the intensive care unit. Throughout the 12-week preoperative period the diarrhea was controlled with Sandostatin, although the dosage had to be progressively increased, up to 900 μg three times a day.
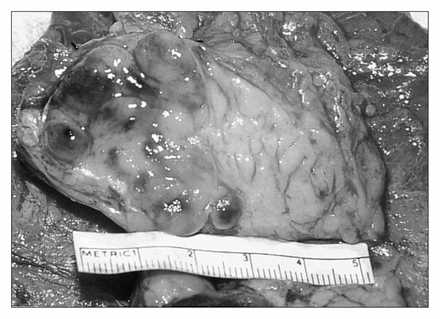
When the empyema resolved the patient underwent resection of the mass in the uncinate process of pancreas through a Whipple pancreaticoduodenectomy (Fig. 2). A right hemicolectomy was also performed to resect a 2 × 3-cm sessile villous adenoma of the ascending colon that could not be removed endoscopically. There were no intraoperative complications.
Cut surgical specimen reveals 3.6 × 3.3 × 3.5-cm circumscribed mass surrounded by normal pancreatic tissue.
The postoperative course was complicated by a prolonged ileus, and intra-abdominal fluid collections that grew Escherichia coli from percutaneous drainage. There was no radiologic evidence of anastomotic leakage, and he responded to antibiotic therapy.
The final pathology report described the pancreatic lesion as consisting of tumour cells with a low nuclear–cytoplasmic ratio, round to oval bland nuclei and neurosecretory-like granules, consistent with an endocrine VIP-secreting tumour. There was no vascular invasion, and all resection margins were free of tumour, although nests of tumour were seen beyond the tumour capsule. Postoperatively the serum VIP level returned to normal and was less than 30 pg/mL. One year postoperatively the patient was clinically well with no diarrhea.
Discussion
The terms watery diarrhea, hypokalemia, achlorhydria (WDHA) syndrome, Verner–Morrison syndrome and pancreatic cholera all describe a watery diarrhea syndrome associated with the overproduction of VIP.
Pancreatic tumours are the primary but not sole origin of VIP secretion.1,2 It may also be produced by neuroblastomas, bronchogenic carcinomas, ganglioneuromas or pheochromocytomas. 3,4 VIP is an ectopic tumour product; it is not normally produced by the islet cells.2 Pancreatic VIP production occurs from a discrete tumour in 80% of cases and from hyperplasia or a microadenoma in 20% of cases.5 In adults, excess VIP production is pancreatic in 90% and extrapancreatic in 10% of cases.2,5 In children 80% of cases are extrapancreatic. Vipomas themselves can be equally benign or malignant.2,6,7
VIP is thought to function physiologically as a local paracrine neuromodulator, which only functions hormonally when produced in excess.5 VIP is a member of the secretinglucagon peptide family. It acts on the gut as a potent secretagogue, using a cAMP (adenosine 3,5-cyclic phosphate)-mediated mechanism,5 among others,1 to produce a massive isosmotic chloride secretion with no mucus or fat that persists during fasting.1,6
Hypokalemia may be severe because large quantities of potassium are drawn into the gut with the chloride secretion. VIP also stimulates renin secretion, augmenting aldosterone production, 1 which is often already stimulated due to volume contraction.
Achlorhydria, part of the complete syndrome, occurs because VIP inhibits gastric mucosal secretion,8 due to a secretin-like action.5 The esophagitis our patient exhibited was not consistent with a typical vipoma. Hypercalcemia due to increased bone resorption is found in 25% to 75% of cases5,9 and abnormal glucose tolerance in 20% to 50% of cases due to a glucagon-like action of VIP.1,8 Flushing, without hypertension is seen in 15% to 20% of cases.6
The diagnosis is suspected on the basis of the clinical symptoms and confirmed with the demonstration of an elevated serum VIP level. This should be drawn during an episode of diarrhea, 8 as levels may be normal when the patient is not having diarrhea.1
Resuscitation of the often severely dehydrated patient is essential. Large quantities of intravenous fluids and potassium may be required. Before octreotide was produced, the voluminous diarrhea often necessitated urgent resection of the tumour in very ill patients because of the intractability of the diarrhea. Sandostatin (octreotide) is a longer-acting analogue of somatostatin that can be given by subcutaneous injection beginning at a dose of 50 to 100 μg every 6 hours.
At least 85% to 90% of patients will experience clinical improvement, allowing a more controlled preoperative workup.1,10–12 Many patients will become tolerant and require higher doses with treatment, or become unresponsive altogether.12 Corticosteroids, formerly first-line medical therapy for control of the diarrhea, may enhance the response to Sandostatin. 1 Other medications that may be considered in the management of the diarrhea include clonidine hydrochloride, indomethacin, lithium, and calcium channel and beta-blocking agents.1,5
Methods of localizing a suspected vipoma preoperatively include imaging with ultrasonography, CT, MRI, angiography or portal venous sampling. 2,5,7 Occasionally, the tumour may be found only by careful inspection at operation.5
The majority of lesions are reported to be located in the distal two-thirds of the pancreas.1 The pancreas should be widely mobilized. Ultrasonography should be used intraoperatively because the malignant mass may be hard to identify. Formal resection is recommended rather than enucleation because of the multifocal nature of the lesion and the difficulty in determining pathologically whether the tumour is benign or malignant. Even obvious metastatic and bulky disease should be debulked since the tumour is often slow growing. Tumour debulking also may provide symptomatic relief.1,5,6,13
Patients with the inherited syndromes of multiple endocrine neoplasia, type I, are more likely to have multiple islet cell tumours.3,10 The use of portal venous sampling has been described but it has been reported that this investigation only confirmed that the dominant tumour was functioning and did not change the operative strategy.2,3
Rebound gastric hypersecretion may occur when the inhibitory effect of VIP on the gastric mucosa is relieved after resection.
Conclusions
Although vipoma is a rare tumour, with a rare constellation of symptoms, it can be treated satisfactorily and even cured by surgical resection. It should be suspected in cases of severe metabolic disturbance due to fasting watery diarrhea. The diagnosis can be confirmed by determination of serum VIP levels and by improvement in diarrhea in response to Sandostatin administration. Somatostatin analogues are extremely effective in preoperative stabilization of these patients and their use should obviate the need to operate prematurely when patients have circulatory instability or concomitant medical problems.
Acknowledgments
We thank Dr. Charlene Leonhardt, Department of Radiology, Sunnybrook Health Science Centre, for reviewing the radiologic findings.
- Accepted February 15, 1995.