Abstract
Persistence of the hypoglossal artery is an unusual congenital abnormality of the carotid arterial system, and the simultaneous occurrence of atheromatous disease in the internal carotid artery and persistent hypoglossal artery is even more uncommon. Carotid surgery in this situation is challenging, and the surgeon must be aware of potential inherent pitfalls. A 74-year-old woman with asymptomatic stenosis of both internal carotid and hypoglossal arteries associated with occlusion of the contralateral internal carotid artery underwent successful revascularization. The anatomy of this unusual lesion and the surgical strategies, which included cranial nerve dissection and mandibular subluxation, are reviewed.
Persistent carotid hypoglossal artery is an unusual vascular anomaly that is reported in less than 0.5% of routine cerebral angiographies. 1,2 It is one of the primitive carotid–basilar anastomoses that, during embryogenesis, supply the posterior cerebral circulation before permeation of the circle of Willis and development of the vertebral arteries. We describe a case of successful revascularization in an asymptomatic patient who had a stenotic, persistent hypoglossal artery associated with an ipsilateral internal carotid artery stenosis and a contralateral carotid artery occlusion. We discuss the operative findings and surgical strategies and review the literature briefly.
Case report
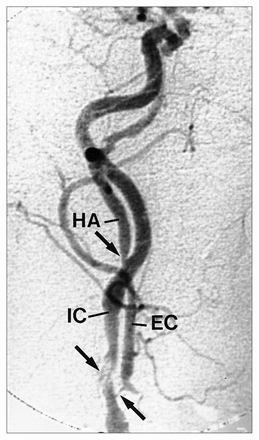
A 74-year-old healthy woman had a history of bilateral asymptomatic carotid bruits. Duplex and continuous Doppler scanning demonstrated an occlusion of the left internal carotid artery and a critical stenosis (reduction of more than 80% of the surface area) of the left external carotid artery. On the right side, both internal and external carotid arteries were severely stenosed. The left vertebral artery was perceived, but the right vertebral artery was not detected. The carotid angiogram confirmed the previous findings but also disclosed an extracranial internal carotid artery branch starting 4 cm above the carotid bifurcation with a 60% (cross-diameter) proximal stenosis (Fig. 1). This side branch was further identified as a persistent hypoglossal artery. The right vertebral artery was aplastic and the left vertebral artery hypoplastic.
Right carotid angiogram. Internal carotid (IC) artery, external carotid (EC) artery and hypoglossal artery (HA) are shown. Arrows indicate area of stenosis.
Since the patient’s cerebral circulation relied on a severely stenotic internal carotid artery with poor collateral circulation, we carried out an elective prophylactic right internal carotid endarterectomy.
Surgery was performed with general anesthesia. Systemic pressure was pharmacologically maintained at 150 mm Hg during the procedure, and a carotid shunt was inserted during the carotid cross-clamping period. The internal carotid stump and the carotid gradient stenosis pressures were measured at 40 and 70 mm Hg respectively. The patient was heparinized (5000 units), and the carotid bifurcation was routinely exposed. However, in order to reach the hypoglossal artery surgical exposure had to be extended. The descendent hypoglossal artery was divided and so were the sternocleidomastoid vein and artery. The hypoglossal nerve was isolated and pulled down to allow better visualization. Then, the common vagal and hypoglossal nerve sheath was divided and the occipital branch of the external carotid artery was divided. All these steps combined with an unusual anterior subluxation of the lower jaw (by the assistant) allowed us to expose the distal internal carotid artery and the proximal hypoglossal artery.
Endarterectomy of the common carotid bifurcation was done first. A calcified atherosclerotic plaque, reducing both internal and external carotid artery lumens by at least 90%, was found extending, in a continuous manner, up to the hypoglossal artery lumen. The endarterectomy was then extended up to the proximal hypoglossal artery. Before terminating the endarterectomy, the common and proximal internal carotid arteriotomies were closed with a saphenous vein patch angioplasty, and the shunt was removed to allow better exposure of the hypoglossal endarterectomy. The hypoglossal endarterectomy ended with a soft distal end point, and the angioplasty was completed up to the proximal hypoglossal artery. Carotid blood flow was re-established and carotid patency confirmed intraoperatively by continuous Doppler assessment. The surgical site was closed in a standard fashion. During removal of the shunt, the cerebral circulation was interrupted for 10 minutes. The patient awoke with a transitory weakness of the left side, but this resolved completely in less than 30 minutes. She left the hospital 4 days later with no central neurologic deficit. Postoperative duplex scanning confirmed the patency of the surgical site. Carotid angiography, performed 4 months after the surgical procedure, showed a well-patent carotid and hypoglossal angioplasty (Fig. 2). At 12-month follow-up, the patient was still asymptomatic with no neurologic sequelae.
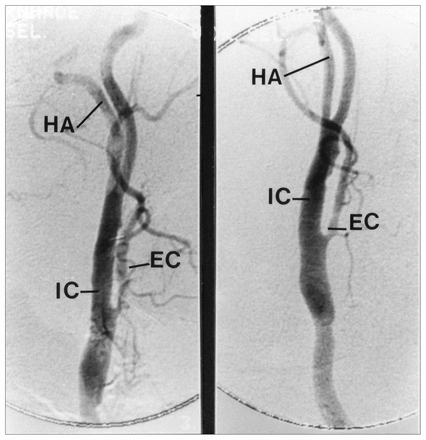
Right carotid angiogram from two different angles confirming patency of angioplasty. IC = internal carotid artery, EC = external carotid artery, HA= hypoglossal artery.
Discussion
Persistent extracranial divisions of the internal carotid artery were first reported in the 19th century, and their embryologic origin was fully described by Padget in 1948.3 Four primitive carotid–basilar anastomoses are known to be occasionally persistent: the trigeminal, the otic, the hypoglossian and proatlantal arteries. The first three anastomoses normally regress once the posterior communicating artery has joined the basilar artery formed by the fusion of both posterior longitudinal neural arteries (Padget’s second stage). Further on, the basilar artery fuses with the vertebral arteries issuing from transverse anastomoses of the 6th cervical segmental arteries. This is followed by the regression of the proatlantal artery (Padget’s third stage).4 The persistence of the hypoglossal artery is the second most frequent of these anomalies, occurring in less than 0.5% of routine cerebral angiographies and is normally associated with hypoplasia or aplasia of vertebral and posterior communicating arteries, as seen in the present case (Fig. 3).2 The artery normally arises from the internal carotid artery at the level of the C1 to C3 vertebral bodies and then travels with the 12th cranial nerve through the hypoglossal canal and the posterior cranial fossa to join the basilar artery.5
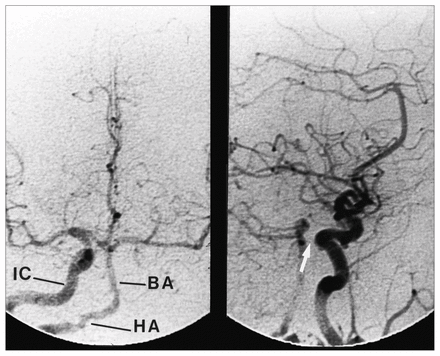
Right carotid and cerebral angiogram showing (left) internal carotid (IC) artery and hypoglossal artery (HA) joining basilar artery (BA) on vertical surface of pons. Arrow (right) points out absence of posterior communicating artery.
Previous reports have cautioned surgeons about the potential risk of major cerebral ischemia during carotid cross-clamping, since the brain stem, cerebellum and ipsilateral cerebral hemisphere are vascularized by a single carotid artery.2,5 The present case perfectly illustrates this situation. Considering the contralateral carotid occlusion and the absence of posterior communicating arteries, the only residual collateral network left was that supplied by a hypotrophic right vertebral artery with no direct communication with the circle of Willis. Even though prophylactic carotid surgery is still debated, it appears to us that revascularizing the left carotid artery of this patient was imperative to avoid an eventual major cerebral deficit. Although the transient hemiparesis in the immediate postoperative period could be attributed to an embolic phenomenon, it remains a concern that the critical dependence of the ipsilateral hemisphere during the temporary flow interruption could have been related to it. Roederer and colleagues6 have reported an annual carotid artery occlusion rate of 46% in patients with greater than 80% carotid stenosis. This patient was, then, exposed to a potential cerebrovascular accident.
Surgical revascularization in this case was particularly difficult. The upward extension of the carotid atheroma to the hypoglossal artery demanded a carotid exposure to the limit of surgical accessibility. The internal carotid artery is usually accessible in the first 4 cm above the common carotid bifurcation. Lesions at the level of C2 or higher normally require either a mandibular subluxation or division of the mandible and the stylomandibular ligament to be safely accessible.7 Fortunately, by dividing the common hypoglossal–vagus junction and ligating the occipital branch of the external carotid artery, along with a gentle manual mandibular subluxation, we were able to achieve satisfactory exposure. In a recent review, Yamanaka and colleagues8 have compiled over 134 cases of persistent hypoglossal artery, of which 28 (20.9%) were associated with cerebrovascular disease. To our knowledge, only one case of isolated hypoglossal endarterectomy for symptomatic atheromatous disease has been reported.9 However, the present case is the first report of combined internal carotid and hypoglossal endarterectomy performed for asymptomatic atheromatous disease.
In conclusion, persistent hypoglossal artery is an unusual feature, but its preoperative recognition is essential in order to minimize neurologic deficits during carotid surgery. The use of a shunt in this situation is strongly advisable, and the surgeon must be familiar with high carotid exposure to handle potential technical difficulties encountered during the procedure.
- Accepted February 15, 1995.