Items 59 and 60
Traumatic rupture of the diaphragm occurs in 3% to 6% of all blunt trauma cases. When intra-abdominal pressure rises rapidly, a large pressure gradient between the abdomen and the thorax is created that results in a burst injury to the muscular diaphragm. Although ruptures of all areas of the diaphragm (left, right, central membranous portion) have been described, 85% occur in the left hemi diaphragm in blunt trauma. Initial chest x-ray is usually abnormal, showing some indistinctness or loss of the left diaphragm silhouette. A nasogastric tube should be placed. The presence of the nasogastric tube in the chest on subsequent x-ray confirms the diagnosis of diaphragmatic rupture (slide A [left]). If the diagnosis cannot be confirmed, barium swallow, chest fluoroscopy, chest computed tomography (CT), nucleotide scans, ultrasound study, and magnetic resonance imaging (MRI) may all be used. None of these tests has proved superior to any other for diagnosis.
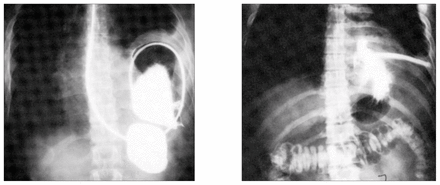
Once the diagnosis is made, the patient should be taken to the operating room for repair of the diaphragmatic defect with permanent sutures through a celiotomy so that all the intra-abdominal viscera can also be examined. Failure to operate may lead to incarceration of an abdominal viscus in the chest with strangulation (slide B [right]). Although the incidence of incarceration after diaphragmatic hernia is unknown, it is believed to be significant. Of all strangulated diaphragmatic hernias, 90% are posttraumatic.
Thoracotomy should only be considered for repair of chronic diaphragmatic hernia, not acute injuries. Although the laparoscope has been advocated for diagnosis of diaphragmatic hernias, laparoscopic repair is unsatisfactory. Retroperitoneal exploration of the left flank has no place in the treatment of this patient.









